Surgery, Gastroenterology and Oncology

|
|
Introduction: Cervical cancer incidence is decreasing in the western world, but the disease remains the most common gynecological malignancy worldwide. About one-third of treatedwomen will have recurrence during follow-up, most often in the first two to three years after the initial treatment, leaving many with limited treatment options and poor prognosis.
Case report: We present a case of a 63-year-old female who was operated for cervical cancer, underwent post-operative radiochemotherapy and had a locoregional recurrence in an unusual location in the presacral region that was successfully treated by stereotactic body radiotherapy.
Discussions: Cervical cancer recurrence management mainly depends on the prior treatments undertaken and on the site and extent of the recurrence. It is particularly difficult in the setting of prior radical hysterectomy and radiochemotherapy, leaving many with limited treatment options and poor prognosis. The therapeutic approach to such cases should be individualized based on the presentation, overall condition, risk factors and limits imposed on the different treat ment modalities. It usually does not involve a single procedure and a single discipline, but is a complex process requiring a thorough interdisciplinary work-up, follow-up and discussions.
Conclusions: The management of cervical cancer recurrences is a complex process requiring a thorough interdisciplinary approach. SBRT can be an effective non-invasive and locoregional cervical cancer recurrence, especially for inoperable cases, possible even in the case of previous radiotherapy in the region, requiring minimal patient effort and potentially significantly improving local control, survival and quality of life.
Introduction
Cervical cancer incidence is decreasing in the western world, but the disease remains the most common gynecological malignancy worldwide, accounting for 6.6 % of all cancers in women (1) and is the fourth deadliest cancer in women (1,2). It has good prognosis when diagnosed in early stage and poor when detected late (3). Cervical cancer treatment choice is determined by the disease stage and includes surgery, radiation therapy, chemotherapy or a combination of these methods (4). About one-third of treated women will have recurrence during follow-up (5), most often in the first two to three years after the initial treatment (6,7), leaving many with limited treatment options and poor prognosis, as surgical removal is not always possible, pharmaceutical therapies are mostly palliative and radiotherapy options for locoregional recurrences usually would have to be a re-irradiation. The type of cervical cancer recurrence is determined by the site of the occurrence and can be defined as either locoregional, distant or lymph node involvement (8).
Case Report
We present a case of a 63-year-old female patient who was operated for cervical cancer, underwent post-operative radiochemotherapy and had a successfully treated locoregional recurrence.
Detailed case description
63-year-old patient is admitted for surgery for proven locoregional recurrence after completed radical treatment. 35 months ago, a class 3 radical hysterectomy with total pelvic lymphadenectomy was performed on a 61-years old female with histologically confirmed cervical cancer. Histopathology report revealed: left ovary – stromal tumor (fibroma-thecoma); cervix – squamous cell carcinoma (3 sm) G3 with perineural, perivasal invasion, emboli in the lymphatics and deep stromal invasion. In total, 21 lymph nodes were dissected and removed, one of which (left) had micrometastasis. Because of the risk factors and high recurrence risk, she was referred for and underwent post-operative radiochemotherapy of the cervical bed and regional (internal and external iliac, obturator, presacral) nodal volumes with 50.4 Gy total dose, 1.8 Gy daily with 5 courses of cisplatin). The technique utilized was linac-based external beam VMAT with daily CBCT image guidance.
Three months post-radiochemotherapy (six months post-op) PET-CT was performed and no pathologic metabolically active lesions were observed. On a new PET-CT study 14 months later, a 17/14/19 mm metabolically active soft tissue lesion in the left presacral region, just outside of the standard high-risk nodal volume treated in post-op RT, was observed (fig. 1).
Figure 1 - PET-CT 22 months post-op – 17/14/19 mm lesion in the left presacral region. SUVmax 16.4

A laparotomy was performed and the described lesion was excised with histological result of foreign body type granuloma. Eight months later, SCC was 1.7 ng/ml (normal range under 1.2 ng/ml) and a new PET-CT was performed, showing the previously described pelvic lesion with increased dimensions of 31/30/37 mm.The mass had grown cranially, already within the post-op radiotherapy treatment volume, with same SUV as before. Disease progression was unequivocally confirmed (fig. 2).
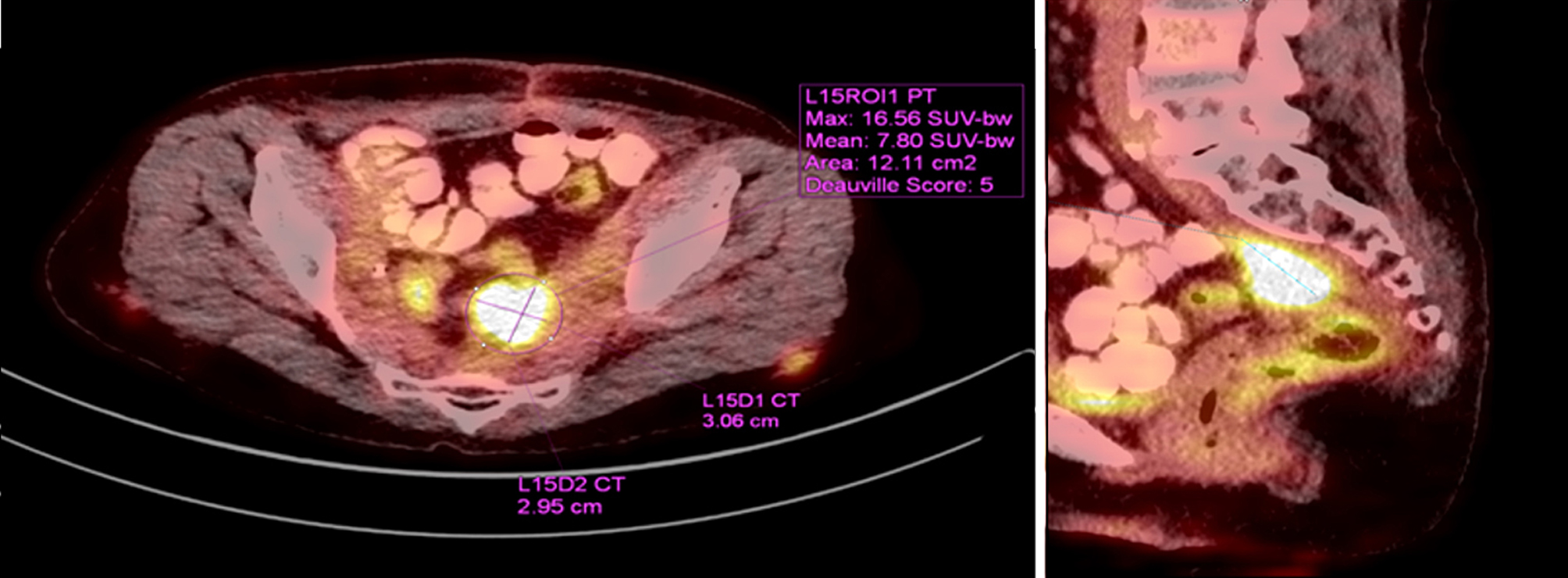
Figure 2 - Confirmed disease progression on PET-CT 29 months post-op - 31/30/37 mm. SUVmax 16.6
MRI was performed, revealing a 3.5 cm lesion, adjacent to the rectum, but not infiltrating it. The patient was referred for consultation for radiosurgery (stereotactic body radiotherapy, SBRT).
She underwent fractionated (5 Gy daily for 5 consecutive days) linac-based SBRT with VMAT IGRT technique. Fusion of PET (from a dedicated new PET-CT performed as part of the treatment planning process) with the planning CT with careful CT-to-CT co-registration was used for target volume delineation and the whole metabolically active volume plus the visible on CT soft-tissue substrate plus 1 cm total margin (reduced to 5 mm toward colon) were included in the planning target volume (PTV) (fig. 3). 6 MV FFF radiation and daily on-board CBCT image guidance with careful consideration of the rectal and lesion volume were used. As part of the VMAT treatment planning the dose was additionally escalated to around 110 % in the metabolically active volume, while in the planning target volume overlapping with colon the dose achieved was 95-105 % of the prescribed dose (fig. 4).
Figure 3 - Fusion of the performed for the SBRT planning PET study set series with the planning CT, with careful CTPET-to-CTplanning coregistration and final target volume delineation

Figure 4 - SBRT treatment plan

PET-CT was performed two months post-SBRT – too early for complete response, because of a suspicious retromandibular lesion that had to be followed up (confirmed to be an unrelated benign process). The treated with SBRT lesion had partial treatment response with decreased dimensions of 29/20 mm and was partially necrotic with decreased SUV (SUVmax 5.3) in comparison with the previous studies (fig. 5).
Figure 5 - Lesion on PET-CT pre-SBRT and 2 months post-SBRT

Shortly after, the patient was referred for surgical consultation and a decision for surgical intervention was taken in discussion with all involved specialists from gynecology, radiotherapy, surgery, pathology and nuclear medicine. Surgery was performed during which presacrally, left from the rectum, a necrotic 3/2 cm formation was identified (fig. 6), separated from adjacent tissues and removed. Histopathology report revealed soft tissues with chronic inflammatory infiltration and fibrosis (chronic non-specific productive inflammation) and no residual tumor cells (fig. 7).

The patient was followed up with another PET-CT at 35 months, revealing no pathological metabolically active lesion in the region of interest, a disease remission.
Discussion
Cervical cancer is the fourth most common cancer in women worldwide with approximately 604 000 new cases and 342 000 deaths in 2020. Around 90% of the new cases and the deaths in 2020 were in low- and mid- income countries. One third of all cervical cancer patients will have recurrence (5), most commonly in the first 3 years after initial diagnosis (6,7).
X-ray computed tomography (CT), magnetic resonance imaging (MRI) and hybrid positron emission tomography with x-ray computed tomography imaging (PET-CT) have a major role in the diagnosis and work-up of cervical cancer recurrence (10,11).
Cervical cancer recurrence has a major impact on the survival outcomes of patients treated for cervical cancer (10), with prognosis dependent on the site of recurrence and the possibility to perform potentially curative therapy.
When lymphogenous metastases are absent at diagnosis, recurrences are usually locoregional, and when lymphogenous metastases are present, recurrences are more common in lymph nodes, at distant or multiple sites (12).
In our case, the patient undertook postoperative radiochemotherapy, even though there was radical
surgical treatment, because of the high recurrence risk due to lymphogenous metastasis (albeit micro) and LVSI + I deep stromal invasion. When a recurrence was found on second follow up PET-CT, the metabolically active soft tissue lesion was nearby but outside of the previously treated with standard radiotherapy volume. The attempt to surgically remove the lesion was unsuccessful - most likely not reached with the standard pelvic surgery approach. On the subsequent PET-CT, the lesion was larger and had grown, mostly in the cranial direction, already partially entering the region of the post-operative radiation treatment. SBRT on a linear accelerator was advised, given the potential and capabilities of the technique for precise targeting of large doses of ionizing radiation with high conformality, advanced imaging guidance and steep dose gradients at the treatment volume margins, especially towards critical organs and structures, given the context of the need to re-irradiate part of the lesion region.
The revealed on the follow-up PET-CT (done only two months after SBRT) partial response (dimensions of 29/25 versus 42/26 pre-SBRT) is insufficient to adequately interpret the response to the performed radiosurgery as the PET-CT was done too early for a clinical complete response, in connection with a followed-up previously observed suspicious retromandibular process that was confirmed to be of completely unrelated benign origin.
The interdisciplinary discussion board concluded that the moment was right for surgical resection because of the current lack of colon infiltration (MRI) and the expected fibrotic changes, that would make a potentially required surgery, in case of incomplete response, more difficult and less successful. The histopathological result from the surgical excision that followed was interpreted as pathological complete response to the performed SBRT.
Conclusions
The management of cervical cancer recurrences is a complex process requiring a thorough interdisciplinary approach. SBRT can be an effective non-invasive and minimally toxic alternative salvage treatment for locoregional cervical cancer recurrence, especially for inoperable cases, possible even in the case of previous radiotherapy in the region, requiring minimal patient effort and potentially significantly improving local control, survival and quality of life.
Author’s contributions
Conceptualization, A.Y., I.P.; methodology, P.IG., B.A.; formal analysis, B.A., P.IG.; investigation, A.Y.,I.K., S.K.; resources, I.P., I.I.; data curation: I.I.; writing—original and draft preparation, A.Y., I.P.; writing—review and editing, S.K..;visualization, I.K.; supervision, A.Y. All authors have read and agreed to the published version of the manuscript.
Conflicts of interest
The authors declare no conflict of interest.
Funding
This research received no external funding.
Ethical statement
Informed consent was signed by the patient.
Data availability
Authors declare that all related data are available concerning researchers by the corresponding author’s email.
References
1. gco.iarc.fr. Lyon, France: GLOBOCAN 2018 - Cancer incidence and mortality worldwide. IARC cancer base: International Agency for Research on Cancer 2019 [cited 2019 May 8] Available from: https://gco.iarc.fr.
2. Patel-Lippmann K, Robbins J, Barroilhet L, Anderson B, Sadowski E, Boyum J. MR imaging of cervical cancer. Magn Reson Imaging Clin N Am. 2017;25(3):635-649.
3. Antunes D, Cunha TM. Recurrent cervical cancer: how can radiology be helpful. OMICS J Radiology 2013;2:6.
4. https://www.nccn.org/professionals/physician_gls/pdf/cervical.pdf
5. de Foucher T, Bendifallah S, Ouldamer L, Bricou A, Lavoue V, Varinot J, et al. Patterns of recurrence and prognosis in locally advanced FIGO stage IB2 to IIB cervical cancer: retrospective multicentre study from the FRANCOGYN Group. Eur J Surg Oncol. 2019;45(4):659-665.
6. Bhatla N, Aoki D, Sharma DN, Sankaranarayanan R. FIGO cancer report 2018 - Cancer of the cervix uteri. Int J Gynaecol Obstet. 2018; 143 (Suppl 2):22-36.
7. Moreira ASL, Cunha TM, Esteves S. Cervical cancer recurrence - can we predict the type of recurrence? Diagn Interv Radiol. 2020; 26(5):403-410.
8. Schieda N, Malone SC, Dandan OA, Ramchandani P, Siegelman ES. Multi-modality organ-based approach to expected imaging findings, complications and recurrent tumor in the genitourinary tract after radiotherapy. Insights Imaging. 2014;5(1):25-40.
9. Sung H, Ferlay J, Siegel RL, Laversanne M, Soerjomataram I, Jemal A, et al. Global cancer statistics 2020: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2021;71(3):209-249.
10. Miccò M, Lupinelli M, Mangialardi M, Gui B, Manfredi R. Patterns of Recurrent Disease in Cervical Cancer. J Pers Med. 2022;12(5):755.
11. Fulcher AS, O’Sullivan SG, Segreti EM, Kavanagh BD. Recurrent cervical carcinoma: typical and atypical manifestations. Radiographics. 1999;19:S103-16; quiz S264-5.
12. Luo Y, Ma X. An Energy-Efficient Test and Predictive Model for Recurrence After Radiotherapy in Localized Intermediate and Advanced Cervical Cancer Were Created Using Thymidine Kinase 1 in Conjunction with Inflammatory Markers and Tumor Markers. Int J Gen Med. 2023;16:5789-5797.
Full Text Sources:
Abstract:
Views: 2441

For Authors
Journal Subscriptions

Dec 2025
Supplements
Instructions for authors
Online submission
Contact
e-ISSN: 2601 - 1700 (online)
ISSN-L: 2559 - 723X
Journal Abbreviation: Surg. Gastroenterol. Oncol.
Surgery, Gastroenterology and Oncology (SGO) is indexed in:
- SCOPUS
- EBSCO
- DOI/Crossref
- Google Scholar
- SCImago
- Harvard Library
- Open Academic Journals Index (OAJI)
Surgery, Gastroenterology and Oncology (SGO) is an open-access, peer-reviewed online journal published by Celsius Publishing House. The journal allows readers to read, download, copy, distribute, print, search, or link to the full text of its articles.
Time to first editorial decision: 25 days
Rejection rate: 61%
CiteScore: 0.2

Meetings and Courses in 2025
Meetings and Courses in 2024
Meetings and Courses in 2023
Meetings and Courses in 2022
Meetings and Courses in 2021
Meetings and Courses in 2020
Meetings and Courses in 2019
Verona expert meeting 2019

Surgery, Gastroenterology and Oncology applies the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits readers to copy and redistribute the material in any medium or format, remix, adapt, build upon the published works non-commercially, and license the derivative works on different terms, provided the original material is properly cited and the use is non-commercial. Please see: https://creativecommons.org/licenses/by-nc/4.0/
Publisher’s Note:
The opinions, statements, and data contained in article are solely those of the authors and not of Surgery, Gastroenterology and Oncology journal or the editors. Publisher and the editors disclaim responsibility for any damage resulting from any ideas, instructions, methods, or products referred to in the content.
 IASGO Society News
IASGO Society News