Surgery, Gastroenterology and Oncology

|
|
Introduction: Choledocholithiasis, the presence of gallstones within the common bile duct, is a challenging medical condition characterized by disruptions in cholesterol, bilirubin, and bile acid metabolism. Patients with choledocholithiasis present with a spectrum of symptoms, from intermittent upper abdominal pain, nausea, and vomiting to jaundice and more severe complications like pancreatitis.
Case report: This case study involves a 63-year-old female who presented at the emergency department with colicky pain, jaundice, and discomfort. An abdominal ultrasound diagnosed choledocholithiasis, leading to an endoscopic retrograde cholangiopancreatography (ERCP). The ERCP procedure was technically challenging, possibly due to the choledocholithiasis of large stones (>1.5 cm). Following the initial ERCP, a follow-up CT scan revealed ongoing bile duct dilation and complications related to the stones, necessitating a second procedure. The reintervention proceeded successfully, and the patient recovered well without complications.
Conclusions: While conventional therapies for choledocholithiasis, such as ERCP and surgical exploration, demonstrate remarkable success, the reappearance of common bile duct stones raises apprehensions. The need for reintervention could be attributed to elements like anatomical complexities during the initial treatment and stone characteristics. Elevating the outcomes and diminishing the necessity for re-interventions hinges upon the refinement of patient selection, preoperative evaluations, and the implementation of a multidisciplinary approach.
INTRODUCTION
Choledocholithiasis, characterized by the presence of gallstones within the common bile duct (1), is a challenging medical condition that demands swift and precise intervention. This ailment not only causes significant discomfort but can also lead to severe complications (2).
The development of choledocholithiasis is often insidious, with patients presenting a spectrum of symptoms ranging from intermittent upper abdominal pain, nausea, and vomiting to jaundice and more serious complications such as pancreatitis (3). Diagnostic procedures for choledocholithiasis typically involve a combination of imaging studies such as ultrasound, computed tomography (CT), magnetic resonance cholangio-pancreatography (MRCP), and endoscopic retrograde cholangiopancreatography (ERCP) (4).
CASE REPORT
A 63-year-old female patient presented at the emergency department of the General Zone Hospital No. 5 in Nogales, Sonora. She had been experiencing colicky pain in the upper right quadrant, associated with jaundice and general discomfort for the past two days. The patient had no significant medical history, no reported allergies, and no comorbidities.
Figure 1 - Initial endoscopic retrograde cholangiopancreatography (ERCP) procedure. (A) ERCP. (B) abdominal computed tomography scan

An abdominal ultrasound diagnosed choledocholithiasis, leading to an ERCP on December 7, 2022 (fig. 1a). During the procedure, we reached the second part of the duodenum, locating the ampulla of Vater in its usual position. However, it had an elongated shape and an extremely narrow Oddi sphincter due to probable dysfunction. Attempts to cannulate it were unsuccessful, leading to a precut from bottom to top, opening the duct. Selective cannulation with a hydrophilic guidewire towards the biliary tract was then successful. We passed contrast medium, visualizing the entire intrahepatic and extrahepatic biliary tract. The extrahepatic bile duct had a diameter of 1.8 cm with several irregularly shaped and faceted filling defects measuring 1.7 cm. We performed sphincterotomy and placed a 10 Fr and 10 cm plastic biliary stent for medium-term fragmentation and drainage safety.
The procedure was completed without incidents. Endoscopy impression: Choledocholithiasis with large elements, placement of plastic biliary stent and dilatation of the extrahepatic biliary tract.
As the ERCP was unsuccessful, a follow-up abdominal CT scan on May 30, 2023, revealed intra-hepatic and extrahepatic bile duct dilation related to choledocho-lithiasis, the presence of a biliary stent in the common bile duct, chronic cholelithiasis, and stone formation in the left renal pelvis leading to hydronephrosis (fig. 1b). The patient was scheduled for biliary tract exploration and left nephrectomy in the same surgical procedure.
Figure 2 - The gallbladder was found with multiple adhesions (a). (b) a longitudinal incision was made in the common bile duct
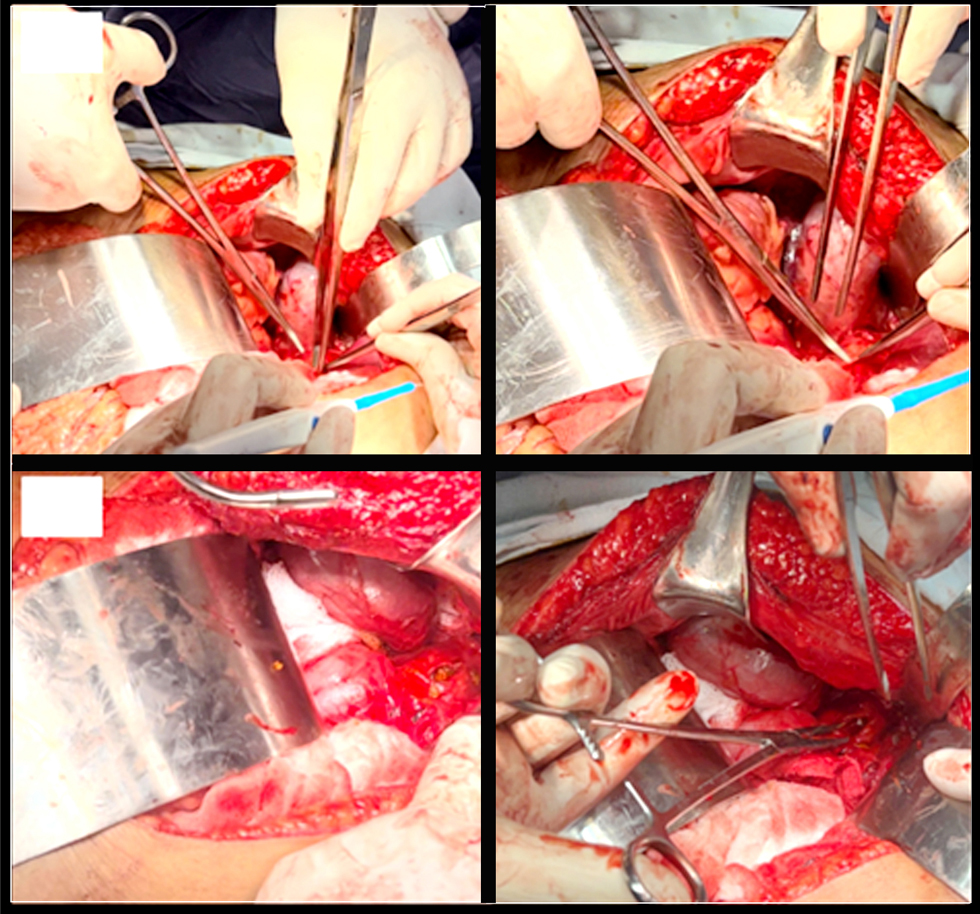
On September 11, 2023, a midline supraumbilical incision was made, followed by dissection through the abdominal layers, gaining access to the peritoneal cavity. The gallbladder was found with multiple
adhesions to the omentum Zuhkle II (fig. 2a), which were resected. The hepatocystic triangle was dissected, and a longitudinal incision was made in the common bile duct (fig. 2b). The biliary tract was explored, and 12 stones, ranging from 1 to 2 cm in diameter, were extracted (fig. 3a). A retrograde and antegrade Fogarty catheter sweep was performed (fig. 3b). A T-tube was placed, and the common bile duct incision was sutured with 3-0 Vicryl simple interrupted stitches (fig. 4a). Trans-tube cholangiography was performed, confirming the contrast medium's proper passage into the duodenum (fig. 4b). The cystic duct was ligated and cut, and the gallbladder was dissected from the vesical bed (fig. 3a). The nephrectomy was then performed, involving the release of the left colon and the identification and ligation of the left renal vein. The Gerota's fascia was incised, and the left kidney was dissected to reach the renal hilum, where the left renal artery was identified, ligated, and cut. Hemostasis was confirmed, four Gelfoam sponges were placed in the renal fossa, a Penrose drain was directed to the left paracolic gutter, and the procedure was completed.

The patient was transferred to the surgical floor and observed for four days. Due to her good recovery, she was discharged with follow-up laboratory tests, which all reported normal parameters.
DISCUSSION
Choledocholithiasis, characterized by gallstones in the common bile duct, presents a significant medical challenge requiring swift intervention. This chronic hepatobiliary ailment is characterized by irregularities in cholesterol, bilirubin, and bile acid metabolism (1). While cholelithiasis is prevalent, choledocholithiasis impacts roughly up to 20 % of individuals with this condition (5,6).
The causes of choledocholithiasis are multifactorial. It often results from the migration of gallstones from the gallbladder into the common bile duct (7). These gallstones obstruct the normal flow of bile and digestive enzymes, leading to a cascade of symptoms. Several risk factors contribute to choledocholithiasis, including age, gender, genetic predisposition, metabolic disorders, dietary habits, and specific medications (8,9).
The management of choledocholithiasis involves a multidisciplinary healthcare approach. Treatment methods may include the common procedure of ERCP, surgical exploration of the biliary tract, and, in some cases, the placement of stents to facilitate bile drainage and stone fragmentation (1). ERCP exhibits a remarkable success rate for intubation, with a corresponding clearance rate of up to 95 % (9). Nevertheless, follow-up studies have revealed recurrence rates of common bile duct stones following treatment, that reach up to 25% (9-11).
The prognosis of choledocholithiasis is generally favorable when diagnosed early and treated promptly. However, choledocholithiasis can lead to severe complications such as acute suppurative cholangitis, pancreatitis, and biliary perforation (2,12). Successful interventions can relieve symptoms and prevent complications. The prognosis may vary depending on the condition's severity, the presence of comorbidities, and the patient's overall health. Close monitoring and follow-up care are often necessary to ensure that patients experience a full recovery and maintain their well-being (13).
The present case illustrates a challenging aspect of choledocholithiasis management. An initial ERCP was performed. The follow-up CT scan revealed continued bile duct dilation and stone-related complications, necessitating reintervention. Several factors could have contributed to the need for a second procedure. These include the complexity of the initial ERCP probably due to large stones (>1.5 cm), an elongated ampulla, and a narrow Oddi sphincter, which may have led to incomplete stone clearance (14,15). Additionally, the nature of the stones might have posed challenges in fragmentation during the initial procedure (15).
To enhance treatment outcomes and minimize reinterventions, healthcare providers should consider better patient selection, improved preoperative assessment, and a multidisciplinary approach to managing complex choledocholithiasis cases. Furthermore, utilizing advanced imaging techniques and novel therapeutic modalities could offer more effective solutions in challenging situations like the one described in this case (16).
CONCLUSION
Standard treatments for choledocholithiasis, including ERCP and surgical exploration, exhibit high success rates. However, the recurrence of common bile duct stones remains a concern. Reintervention may result from factors like anatomical challenges during the initial treatment and the nature of the stones (diameter >1.5 cm). To enhance outcomes and reduce reinterventions, improved patient selection, preoperative assessment, and a multidisciplinary approach are crucial.
Acknowledgements
The authors express their gratitude to the Instituto Mexicano del Seguro Social (IMSS) for permitting access to facilities during this research.
Conflict of interest and funding: None.
Ethical statement
Written informed consent was obtained from the patient of this case report.
REFERENCES
1. Molvar C, Glaenzer B. Choledocholithiasis: Evaluation, Treatment, and Outcomes. Semin Intervent Radiol. 2016;33(4):268-76.
2. Akmal AM, Putra BP, Darmaningrat C, Nariswari I, Srigede LD, Budyono C. Management of Cholelithiasis with Concomitant Choledocholithiasis. Acta Med Indones. 2022;54(1):151-7.
3. Minguez A, Ladron P, Martinez S, Del Val A, Nos P, de-Madaria E. Predictive model of persistent choledocholithiasis in patients with acute biliary pancreatitis. Gastroenterol Hepatol. 2023;46(4):297-304.
4. Narula VK, Fung EC, Overby DW, Richardson W, Stefanidis D, Committee SG. Clinical spotlight review for the management of choledocholithiasis. Surg Endosc. 2020;34(4):1482-91.
5. Li S, Guizzetti L, Ma C, Shaheen AA, Dixon E, Ball C, et al. Epidemiology and outcomes of choledocholithiasis and cholangitis in the United States: trends and urban-rural variations. BMC Gastroenterol. 2023;23(1):254.
6. De Silva WSL, Pathirana AA, Wijerathne TK, Gamage BD, Dassanayake BK, De Silva MM. Epidemiology and disease characteristics of symptomatic choledocholithiasis in Sri Lanka. Ann Hepatobiliary Pancreat Surg. 2019;23(1):41-5.
7. Costi R, Gnocchi A, Di Mario F, Sarli L. Diagnosis and management of choledocholithiasis in the golden age of imaging, endoscopy and laparoscopy. World J Gastroenterol. 2014;20(37):13382-401.
8. Zhang J, Ling X. Risk factors and management of primary choledocholithiasis: a systematic review. ANZ J Surg. 2021;91(4):530-6.
9. Wu Y, Xu CJ, Xu SF. Advances in Risk Factors for Recurrence of Common Bile Duct Stones. Int J Med Sci. 2021;18(4):1067-74.
10. Parra-Membrives P, Martinez-Baena D, Lorente-Herce JM, Jimenez-Riera G, Sanchez-Galvez MA. Choledocholithiasis recurrence following laparoscopic common bile duct exploration. Cir Esp (Engl Ed). 2019;97(6):336-42.
11. Konstantakis C, Triantos C, Theopistos V, Theocharis G, Maroulis I, Diamantopoulou G, et al. Recurrence of choledocholithiasis following endoscopic bile duct clearance: Long term results and factors associated with recurrent bile duct stones. World J Gastrointest Endosc. 2017;9(1):26-33.
12. Chhoda A, Mukewar SS, Mahadev S. Managing Gallstone Disease in the Elderly. Clin Geriatr Med. 2021;37(1):43-69.
13. Sugimoto S, Hattori A, Maegawa Y, Nakamura H, Okuda N, Takeuchi T, et al. Long-term Outcomes of Therapeutic Endoscopic Retrograde Cholangiopancreatography for Choledocholithiasis in Patients ³90 Years Old: A Multicenter Retrospective Study. Intern Med. 2021; 60(13):1989-97.
14. Almadi MA, Eltayeb M, Thaniah S, Alrashed F, Aljebreen MA, Alharbi OR, et al. Predictors of failure of endoscopic retrograde cholangiography in clearing bile duct stone on the initial procedure. Saudi J Gastroenterol. 2019;25(2):132-8.
15. Sbeit W, Kadah A, Simaan M, Shahin A, Khoury T. Predictors of recurrent bile duct stone after clearance by endoscopic retrograde cholangiopancreatography: A case-control study. Hepatobiliary Pancreat Dis Int. 2022;21(1):50-5.
16. Guo T, Wang L, Xie P, Zhang Z, Huang X, Yu Y. Surgical methods of treatment for cholecystolithiasis combined with choledocholithiasis: six years' experience of a single institution. Surg Endosc. 2022; 36(7):4903-11.
Full Text Sources:
Abstract:
Views: 6938

For Authors
Journal Subscriptions

Dec 2025
Supplements
Instructions for authors
Online submission
Contact
e-ISSN: 2601 - 1700 (online)
ISSN-L: 2559 - 723X
Journal Abbreviation: Surg. Gastroenterol. Oncol.
Surgery, Gastroenterology and Oncology (SGO) is indexed in:
- SCOPUS
- EBSCO
- DOI/Crossref
- Google Scholar
- SCImago
- Harvard Library
- Open Academic Journals Index (OAJI)
Surgery, Gastroenterology and Oncology (SGO) is an open-access, peer-reviewed online journal published by Celsius Publishing House. The journal allows readers to read, download, copy, distribute, print, search, or link to the full text of its articles.
Time to first editorial decision: 25 days
Rejection rate: 61%
CiteScore: 0.2

Meetings and Courses in 2025
Meetings and Courses in 2024
Meetings and Courses in 2023
Meetings and Courses in 2022
Meetings and Courses in 2021
Meetings and Courses in 2020
Meetings and Courses in 2019
Verona expert meeting 2019

Surgery, Gastroenterology and Oncology applies the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits readers to copy and redistribute the material in any medium or format, remix, adapt, build upon the published works non-commercially, and license the derivative works on different terms, provided the original material is properly cited and the use is non-commercial. Please see: https://creativecommons.org/licenses/by-nc/4.0/
Publisher’s Note:
The opinions, statements, and data contained in article are solely those of the authors and not of Surgery, Gastroenterology and Oncology journal or the editors. Publisher and the editors disclaim responsibility for any damage resulting from any ideas, instructions, methods, or products referred to in the content.
 IASGO Society News
IASGO Society News