Surgery, Gastroenterology and Oncology

|
|
Introduction: Acute appendicitis is one of the most frequent and challenging surgical emergencies, and can lead to perforation and peritonitis, which are concomitant with high mortality and morbidity. The epidemiology and natural course of acute appendicitis are still obscured. Therefore, the aim of the study is to determine the prevalence of appendicitis among patients registered in Dammam Medical Center as a retrospective cohort study. The data was collected from admission records in surgical department of DMC during the period October 2020 – October 2023.
Material and Methods: A total number of 806 patients attending surgical ward with acute appendicitis were collected from records of the hospital. The prevalence of acute appendicitis during the study years was 57.3%. The prevalence of acute appendicitis was (57.3%), (63.8%) were male while (36.2%) were female. The prevalence peaks among both gender was adult from 20-45 age, and the prevalence has decreased with increasing of age in both males and females. The prevalence of acute appendicitis with perforation was significantly higher among male 109 (71.2%).
Results: Accuracy of CT scan for detecting appendicitis was more than half, while only near third showed U/S accuracy, the majority of CT (97%) showed true operative finding compared to 80% for clinical diagnosis and 72% for U/S. On the other hand, the prevalence of appendicitis without perforation was significantly higher among female 139(58.6%). Three years' period of study (2020-2023) showed yearly prevalence variation of appendicitis with peak increase during the year (2020-2021). There was significant statistical association between patients' age groups and gender in the occurrence of acute appendicitis (p-; 0.008, 0.001 respectively).
Conclusion: In this study, obvious differences were observed in the prevalence of acute appendicitis for age groups (20-45) with higher rate among male.
Introduction
Acute inflammation of the appendix is a frequent emergency in surgery department, distressing 17.7 million individuals every year globally. The age range of 15 to 19 is the one where it is most common. With a high mean hospital cost and subsequent national yearly costs, acute appendicitis has a substantial healthcare liability (1). The traditional practice of conducting emergency surgery on all patients with suspected appendicitis has increasingly been replaced by more prospective tactics for the management of acute appendicitis. This traditional line of treatment was accepting a high rate of negative appendectomy to avoid possible perforation (2). The most frequent cause of acute abdomen is appendicitis. It is an abrupt, acute inflammation of the vermiform appendix that is accompanied by nausea, vomiting, and constipation. The lower right quadrant is often the site of the discomfort. The cause of appendicitis is still unidentified and multifaceted. Numerous factors have been proposed as potential causes of the illness, including smoking, air fumes, mechanical blockage, and genetic susceptibility (3).
With up to 16% of the people needing appendectomy, the incidence of appendicitis appears to have increased significantly in the first half of this century, especially in Europe, America, and Australasia. Different nations have different rates of acute appendicitis. There have been reports of declining acute appendicitis rates in Europe and the United States. These nations have had a sharp decline in the incidence over the previous 30 years, with a lifetime risk of 6.7% for women and 8.6% for men of appendectomy. Nonetheless, it seems that in rising nations, the frequency is expanding (4).
Acute inflammation of appendix had a crude occurrence of 86 cases per 100,000 people annually. A delayed diagnosis increases the risk of surgery, as well as the costs associated with care, morbidity, and mortality. Even though it is so widespread, diagnosing it is still challenging. While most practitioners believe that prompt identification of acute appendicitis before complications arise is essential for patient care, this is challenging (5).
The increased occurrence of appendicitis in recently industrialised nations could point to an appendicitis epidemic outside of Western nations. In order to reduce appendicitis morbidity and death, the clinical infrastructure in newly industrialised nations might need to be more effective. Moreover, comparing the prevalence of appendicitis in recently industrialised and Western nations may provide insights into the environmental factors that underlie appendicitis. Public policy efforts can be formed to change environmental exposures that prevent appendicitis by identifying environmental causes of appendicitis. (6)
Despite being a prevalent surgical illness, the epidemiology of acute appendicitis is poorly understood. Ensuring adequate patient treatment requires improving the diagnostic route, which is the cornerstone for reducing the rate of negative appendectomy and the risk of diagnosis mistake. It is also essential to distinguish between non-complicated and appendicitis with adverse effect. Thus, the purpose of this investigation was to ascertain the prevalence of appendicitis among patients admitted to Dammam Medical Center Through emergency room (ER) to Surgical Ward during the period between October 2020 and October 2023.
Materials and method
The study was a retrospective cohort study, relied on data that had been collected through medical records. This study included all patients with appendicitis registered for treatment at Dammam Medical Center through ER to Surgical Ward district from October 2020 to October 2023. The Dammam Medical Center (DMC) in Dammam, Saudi Arabia is the main referral hospital that provides health services to the population from the following geographical areas (Saudi, India, Pakistan, Bangladesh, and Egypt).
Inclusion criteria
All appendicitis patients adult more than 14, both male and female, all races and ethnics who visit the department of surgery for any complain were included.
Exclusion criteria
Pregnant woman and child less than 14.
Data analysis
The data were analyzed using (statistical package for social software) SPSS version (20), frequencies and percentages for categorical data. Comparisons were done with the Chi-square test and p-value level.
Results
A total of 806 patients were included in this study, during the period from October 2020 to October 2023. Regarding age distribution, 158 patients (19.6%) were at the age of 14- 20 years, 599 patients (74.3 %) were between 20 - 45 years old and 49 patients (6.1 %) were more than 45 years. Mean age of the patients was 28.5±10.1 years. The most frequent age among the studied group was between the age from 20 to 45 years (table 1, fig. 1).
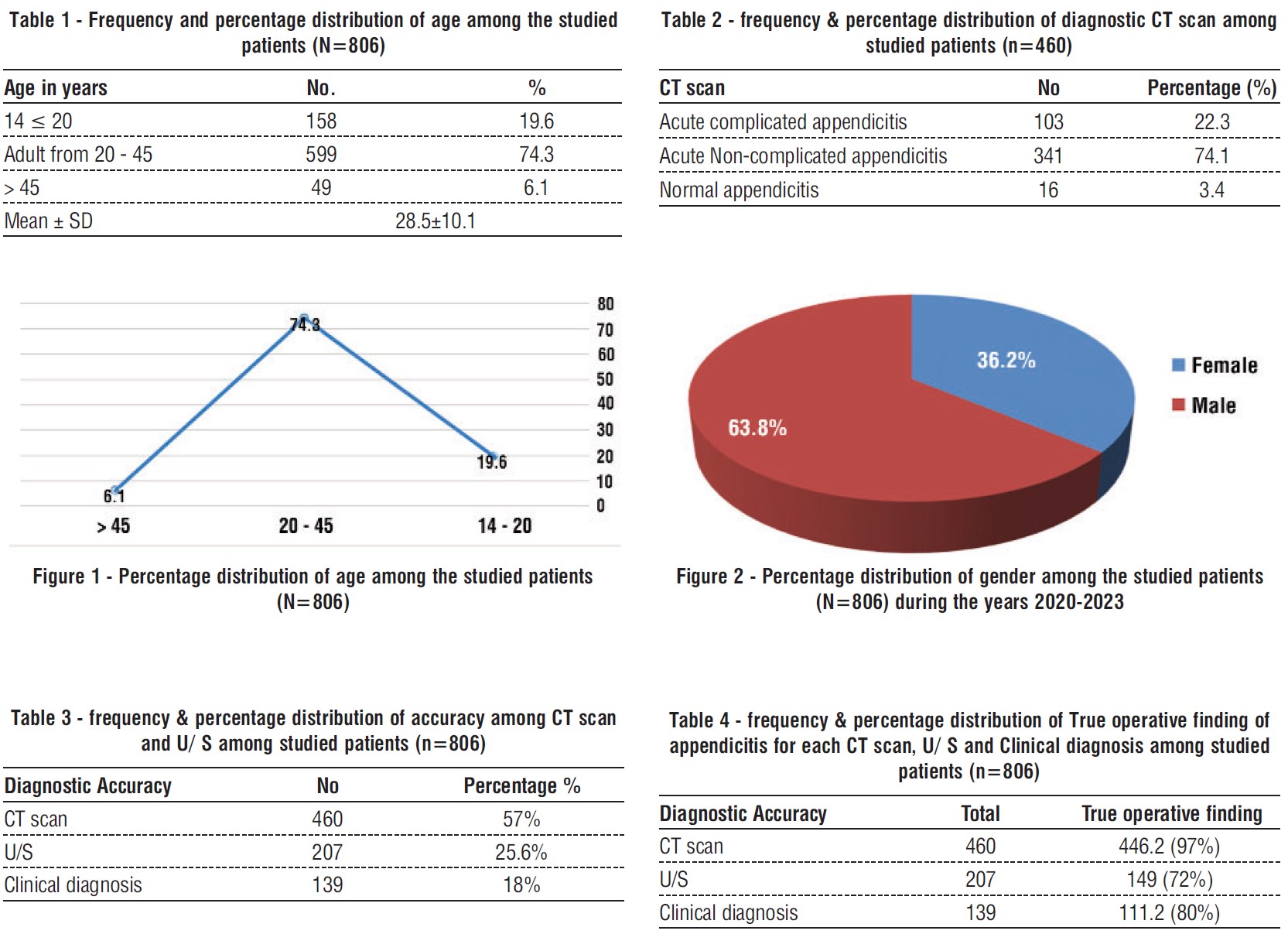
Out of 806 patients, 514 (63.8%) were male while remaining 292 patients (36.2%) were female. There were 460 (57%) confirmed diagnosis of appendicitis through Computed Tomography (CT) scan, out of the number of patients diagnosed with CT scan, there were 103 (22.3%) with acute complicated appendicitis, while 341 (74.1%) reveal acute non-complicated appendicitis and 16 (3.4%) were normal (fig. 2, table 2).
As regard the accuracy among the diagnostic procedure, the accuracy of CT scan was 57% while Ultrasound (U/S) showed 25.6% accuracy. The most accurate for true operative finding of appendicitis was 97% for CT scan, 72% for U/S, while 80% for clinical diagnosis (tables 3, 4).
Out of 460 (the total number of patients undergoing CT), 446.2 showed true operative finding, out of 207 undergoing U/S, 149 matched with operative finding, while 111.2 out of 139 diagnosed clinically were of true operative finding match (fig. 3) (3).
Figure 3 - Percentage distribution comparison between total and true operative finding of appendicitis for each CT scan, U/ S and Clinical Diagnosis

Concerning the management of appendicitis, the results showed that there were 712 (88.3%) of patients treated with open appendectomy, 32 (3.9%) treated with conservative management (abscess, mass, comorbidity), while 62 (7.7%) treated with Laparoscopic appendectomy (table 5).
Table 5 - Frequency and percentage distribution of Management among studied patients (N=806)

Fig. 4 revealed that, the total patients attending the surgical wards were 806 out of them 462 (57.3%) patients diagnosed with acute appendicitis as collected from records of the hospital. Cases were divided as; 201 (43.5%) acute appendicitis without perforation, 153 (33.1%) acute appendicitis with perforation, 72 (15.5%) normal appendicitis, 23 (4.9%) appendicular mass and 11 (2.3%) were appendicular abscess.
Figure 4 - Frequency and percentage distribution of prevalence of appendicitis with and without complications among studied patients (N=462) during the years 2020-2023.
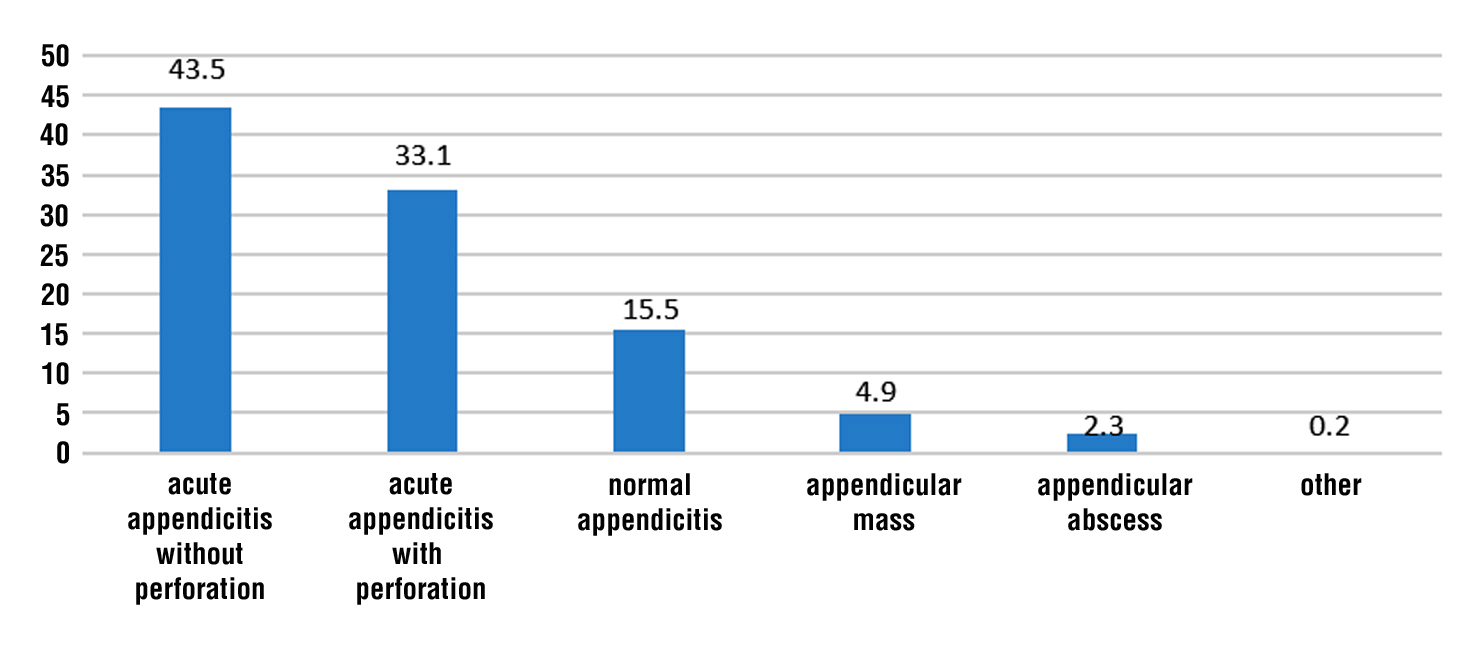
Table 6 - Prevalence of Appendicitis among studied patients according to the status (N=806)

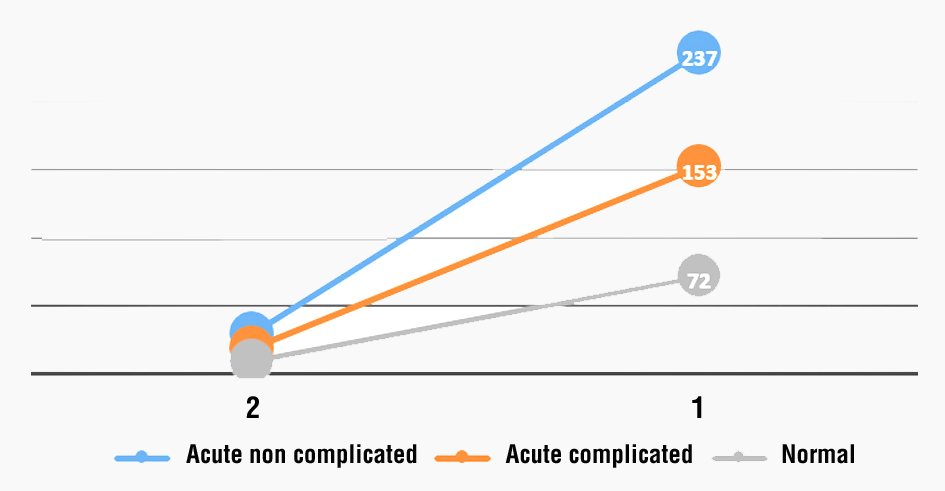
Table 6 and fig. 5 show that the prevalence of acute non- complicated appendicitis were 237 (51.2 %) while acute complicated were 153 (33.1%) and 72 (15.5%) were normal.
The distribution of acute appendicitis regarding age groups, as regard the number of non-perforated appendicitis, 40 (25.3%) of patients were at the age of 14- 20, and the most frequent of recorded patients were the age group from 20 to 45 years 180 (30.0%). Regarding the perforated appendicitis, 33(20.8%) of studied patients were at the age of 14- 20, while the largest number 106 (17.6 %) of studied patients were at age group from 20 to 45 years. It was observed that the number of patients decreased when the patients become older (table 7).
Figure 5 - Prevalence of Appendicitis among studied patients according to the status (N=806)
Using Chi square test, it was found that, there was statistical significant association between patients' age groups and the occurrence of acute appendicitis of perforated and non-perforated (p-.0.02*, 0.001*) respectively.
Table 8 shows that the highest number of appendicitis cases (280) occurred in the 2021-2022 study period, followed by 2022-2023 (276) and 2020-2021 (250). While the highest and lowest years differ by only 24 cases, there is a slight increase in cases over the first two years followed by a decrease in the third year.
Table 7 - frequency & percentage distribution of appendicitis regarding age groups (N=806)
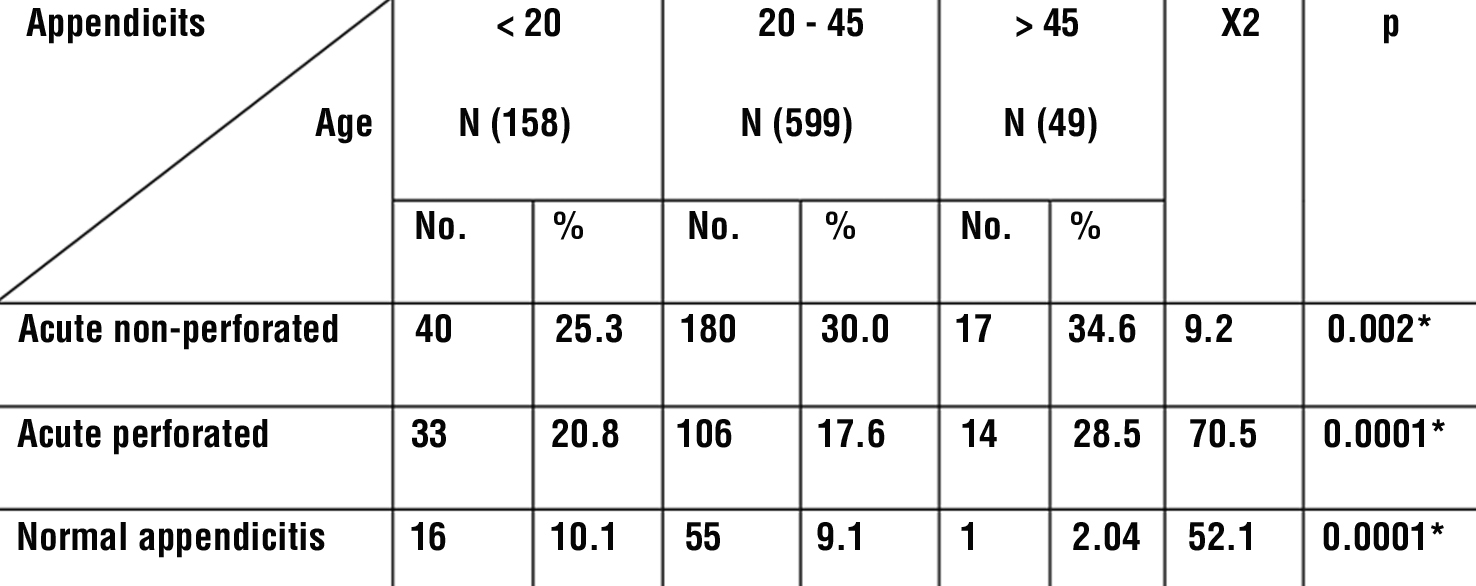
Table 8 - Distribution of acute appendicitis during the study years 2020- 2022 (n=806).
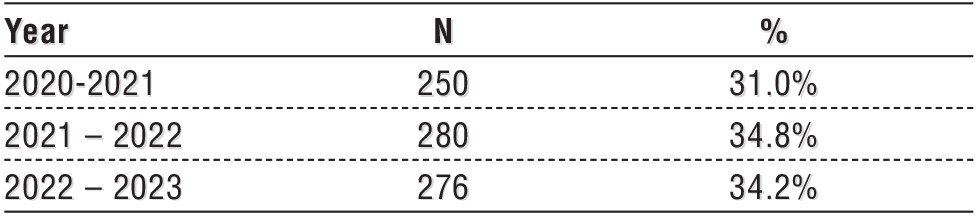
Fig. 6 clarified that the number of patients with acute appendicitis is increasing yearly starting from 100 at the year 2019 to 301 at the year 2021. And the highest frequency 301 (37.3%) was observed during the year from 2020-2021.
Figure 6 - Distribution of acute appendicitis during the study years 2020-2022 (n=806).
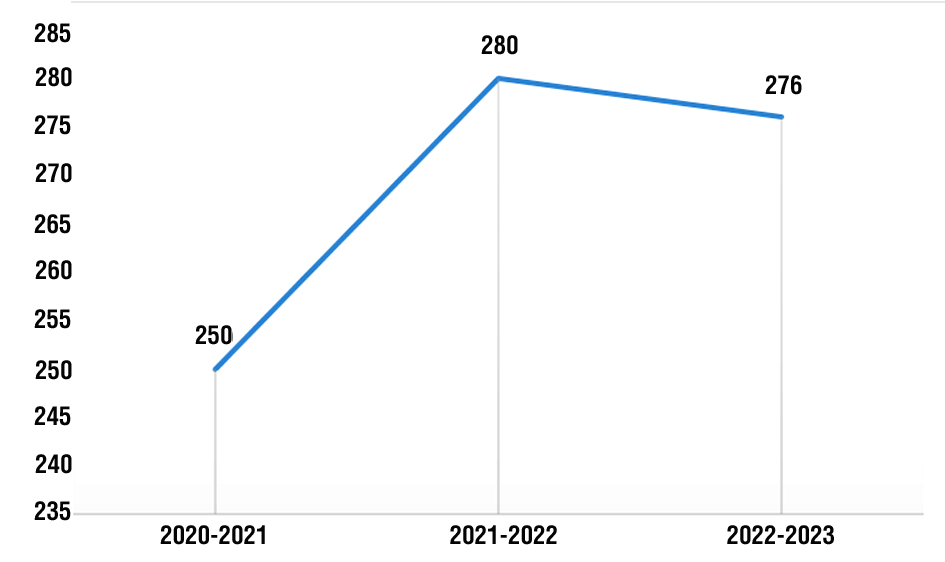
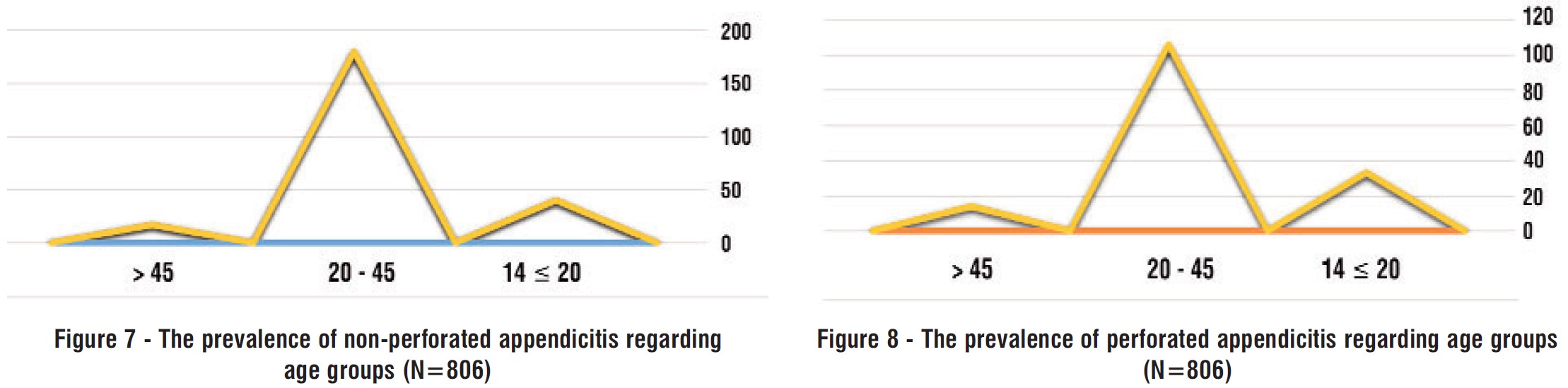
Fig. 7 showed that the most prevalence of nonperforated appendicitis was among the age group from 20 to 45. As shown in fig. 8 that the most prevalence of acute perforated appendicitis was between the age from 20 to 45 years.
As shown in table 9, it was found that, the prevalence of acute appendicitis without perforation was significantly higher among female 139 (58.6 %). On the other hand, the prevalence of acute appendicitis with perforation was significantly higher among male 109 (71.2%). The prevalence of normal appendicitis among female and male were 30 (41.6%), 42 (58.3%) respectively.
Table 9 - Distribution of acute appendicitis according to gender among the studied patients (N=806) during the years 2020-2023
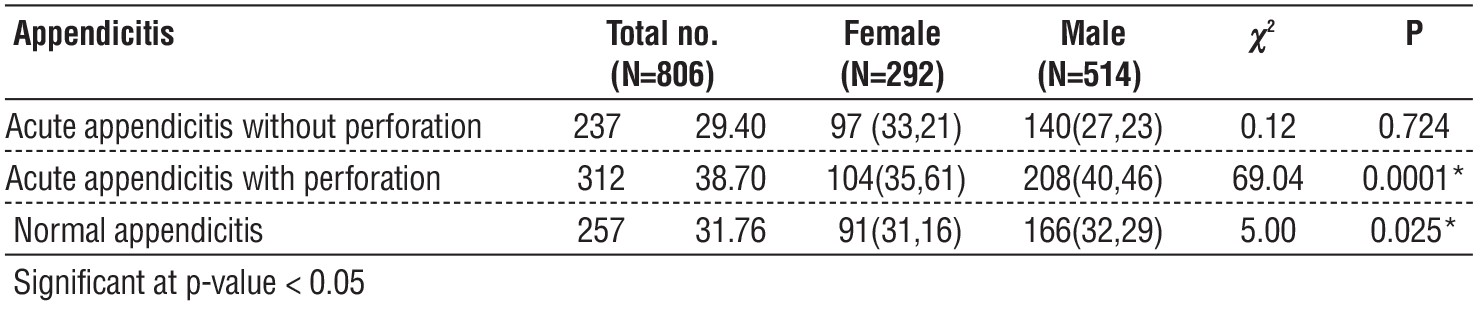
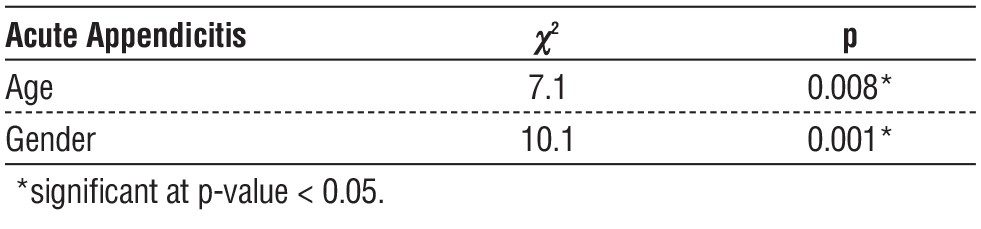
Using Chi square test, table 9, revealed that, it was found that, there was significant statistical association between patients' age groups and gender in the occurrence of acute appendicitis (0.008*,0.001* respectively).
According to table 10 there is a statistically significant association between age and acute appendicitis. This means that the prevalence of acute appendicitis is likely not the same across all age groups. It also indicates a statistically significant association between gender and acute appendicitis. This suggests a difference in the prevalence of acute appendicitis between males and females.
Table 10 - Association between Prevalence of acute appendicitis with age and gender
Discussion
Acute inflammation of the appendix is one of the most frequent surgical emergencies in the world; appendicitis places a significant strain on contemporary healthcare systems. Due to the high prevalence of appendicitis epidemics in adults and children globally, prior researches on these outbreaks has been concentrating on incident cases. Since the 1990s, the disease's pooled incidence has decreased in high-income areas and nations, while it has climbed in recently industrialized nations (7). Disability-adjusted life-years, a complete measure of premature death and disability, are a useful metric that should be analyzed across geographical locations, even though appendicitis is also linked to a higher risk of morbidity and mortality. Appendicitis continues to be a clinical emergency in spite of medical advancements in diagnosis and treatment (8), therefore, the current study aimed to determine the prevalence of appendicitis among patient admitted to Dammam Medical Center.
The present study included 806 patients. Their age varied from 14 years to more than 60 years. The mean age of the patients was 28.5 ± 10.1 years. The age distribution in our study revealed that, the majority of the studied patients were between the adult age group from 20-45 years. While, about one third were at the age of 14-20 years. In our investigation, the prevalence of acute inflammation of appendix was comparable to Körner et al., (1997) (9). They performed a large cohort on incidence of acute inflammation: non-perforated and perforated types of appendicitis: age- and sex specific investigation, which reported that the highest incidence was detected in young adults. For the ages from 13 to 40 years, males were the most frequent reported in their research. This study may be corresponded with the study of Schildberg et al., (2022) about acute appendicitis, diagnosis, therapy and complications on 19,749 patients, which reported that the age distribution showed a substantial rise in cases aged 18-29 years (41.9%) and 30-39 years of age (16.7%) (10).
Regarding gender distribution, the current study finding showed that, (63.8%) of the studied subjects were male and more than one third of them were female, this study matched with Parsons et al., (2022) study which revealed that out of 776 participants, (37%) were female and (63%) were male (11). In addition, there was an agreement with another study that on a diagnostic score for acute appendicitis demonstrated that 111 patients (41.6%) were females and 156 (58.4%) were males (12).
In order to diagnose appendicitis and lower the risk of unsuccessful appendectomies, imaging in preoperative stage is crucial. The first-line imaging test for adult appendicitis diagnosis is CT of contrast-enhanced type, following the American College of Radiology Appropriateness Criteria. Because CT is so accurate—its range of sensitivities is 85.7% - 100% and its range of specificities is 94.8% -100%—it is frequently used to diagnose appendicitis and is a better diagnostic tool than compression ultrasound. (13). The current study revealed that the accuracy of CT scan for detecting appendicitis was more than half while only near third U/S accuracy. Furthermore, more than half of the studied patients underwent CT scan and revealed that 22.3 % of the studied subjects confirmed acute complicated appendicitis, near three quarters were acute non complicated and the remaining were normal, which was consistent with Avanesov et al., (2018), while using severity index of combined clinical and radiological appendicitis for studying diagnostic prediction of complicated appendicitis. They summarized that most patients experience CT scan in the pre-operative stage (74.6–97.9%), and pathological tissue biopsy proven complication of appendicitis in (51%), based on CT (14). Furthermore, Syed & Naji, (2021) performed a backdated investigation of children acute inflammation of appendix cured with laparoscopic appendectomies at a one center in Dubai. They disclosed that abdominal CT scan was conducted to 44.6% of the cases. Acute inflammation of appendix was identified on CT examination in all patients, and visualization of free fluid was detected in 64% of cases (15).
Regarding evaluating the accuracy of CT scan versus U/S examinations, and clinical diagnosis, our study showed high accuracy of CT in diagnosing appendicitis (more than half of the studied subject) while only near third for ultrasound accuracy, the majority of CT (97%) show true operative finding compared to 80% for clinical diagnosis and 72% for U/S. High accuracy is one of the advantage of CT, however, it is an expensive tool and takes time, while U\S shows operative dependent and less accuracy. Otherwise, clinical diagnosis is considered easy with direct decision, although it can lead to misdiagnosis with mickle diveticulum and ectopic pregnancy or other pathology.
This study was consistent with Crocker et al., (2020) about U/S and CT in the Diagnosing acute inflation of appendix according to STARD Guidelines, which showed that 13.7% and 95.6% were accurate for U/S and CT respectively. They reported significant rates of negative appendectomy 17.7% and 3.3 % for U/S and CT respectively and concluded that CT is the chosen imaging examination for assessing appendicitis in no obstetric adult cases (16).
As regard appendicitis prevalence amongst the studied patients, the current study finding showed that the higher prevalence was acute non-complicated appendicitis (more than half of the studied subjects), and while more than one third of cases showed acute complicated appendicitis. This study matched with Baghdadi, Metwalli, & Abdelhamid, (2019) that the participants were divided into (57% and 43%) patients with non-complicated and complicated appendicitis respectively (17). As well as Potey et al., (2023) who clarified that perforation of appendicitis was found in 13.8% of the studied cases of acute appendicitis (18).
In the current study, we discovered a strong association between the age of the patients and the frequency of appendicitis, based on this study, 20-45 years of age was susceptible for appendicitis, this may be explained by that appendicitis can be found in all ages but mostly in span of age 20 to 45 years old. 20-40 years old is productive age with many efforts that can affect way of living and dietary life style. This study matched with Weinandt et al., (2020), about Appendicitis as a Severe Disease in Elderly Patients, who reported that the prevalence of appendicitis increases in patients younger than 40. (19) A similar results obtained by Qasim et al., (2014), who proven that, out of 267214 patients (80.1%) were between 26-40 years of age (12). A different research by Thomas (1998) in Saudi Arabia, clarified that acute appendicitis is more prevalent in people between the ages of 10 and 29. Another study by Mungadi et al. (2004) in Nigeria revealed that acute appendicitis is more common in people between the ages of 20 and 29 (20,21).
Three years' duration of research (2020-2023) revealed yearly prevalence variation of acute inflammation of appendix with ultimate increase during the year from (2020-2021), during the onset of Covid 19 global infection, the reasons underlying maybe attributed to COVID-19 quarantine and avoidance of infection leading to late presentation after symptom onset. The higher post-surgery site contamination and fluid collection, and rising septic shock, is a finding consistent with Kariya et al., (2022) addressing occurrence of complication in appendicitis during the pandemic of COVID-19 who reported that such complication frequency was considerably greater throughout the pandemic (22).
As well as Scheijmans et al., (2021) about influence of the pandemic COVID-19 on rate and severity of acute inflammation of appendix which was a comparison between 2019 & 2020. It summarized that, during the pandemic, a substantial greater percentage of appendicitis with complications was detected. 61.1% of patients compared to 56.2% reported symptoms lasting longer than 24 hours, with a p-value of 0.048. Presentation during the first wave of the COVID-19 pandemic was linked to a greater likelihood of complex appendicitis even if prehospital delay was taken into account. Patients who appeared more than 24 hours following the start of the pandemic were significantly older in age and had more postoperative complications (23).
The variation in the incidence of acute appendicitis by age and sex is one of the most important epidemiological characteristics of appendicitis. The current study's findings showed a substantial correlation between the patients' gender and the prevalence of acute appendicitis (0.001*). Bar???k & Bener, (2020), support this finding and Gignoux et al., (2018) who found that gender had a significant relation to incidence of appendicitis (6,24).
Additionally, it was noted that 109 males had a substantially greater rate of acute appendicitis with perforation (71.2%). Instead, the appendicitis prevalence without perforation was significantly higher among female 139 (58.6 %). This may be due to the anatomical difference between male and female as the appendix wall in male has many lymphoid tissue than in female. Appendicitis also found in people who consume low fiber food, or irregular time of eating, which can subsequently lead toappendicitis. This was in line with other research from Yemen, Nigeria, Iran, Ghana, and Canada, which found that appendicitis was more common in men than in women (3,25-28). Additionally, Albahadili (2016) conducted research in Azizyah, Iraq, regarding the impact of age, gender, and seasonal variation on appendicitis. They reported that, with a male to female ratio of 1.27:1, appendicitis was far more prevalent in men (56%) than in women (29). The results of the current study may differ from those of a study carried out in Tehran by Noudeh et al., which revealed that appendicitis is more prevalent in males between the ages of 21 and 30, while it is more common in girls between the ages of 11 and 20 (26).
Conclusion
A total of 806 patients were included in this study, during the period of October 2020 to October 2023. There was significant statistical association between patients' age groups and gender in the occurrence of acute appendicitis. The prevalence of acute appendicitis among patient admitted to Dammam Medical Center during the 3 years was (57.3%), the majority were between 20 - 45 years and near two third were male with significant higher prevalence of acute appendicitis with perforation. Then again, the prevalence of appendicitis without perforation was significantly higher among female. CT scan for detecting appendicitis showed higher accuracy with marked true operative finding; hence, CT and clinical diagnosis are the more efficient method in diagnosing appendicitis. The peak year prevalence was (2020-2021), during and maybe related to the onset of Covid 19.
Authorship
All persons listed as authors have been actively involved in one or more key aspects of the reported study. All authors confirm that they have met the criteria for authorship as established by the International Committee of Medical Journal Editors (http://www.icmje.org). Full responsibility for the content of articles lies with the authors.
Conflicts of interest and source of funding
The authors declare no conflicts of interest.
Ethical approval
This research is in accordance with the ethical standards of the responsible committee on human experimentation (institutional and national) and with the Helsinki Committee for Human Rights.
References
1. Narsule CK, Kahle EJ, Kim DS, Anderson AC, Luks FI. Effect of delay in presentation on rate of perforation in children with appendicitis. Am J Emerg Med. 2011;(8):890-3.
2. Bachur RG, Lipsett SC, Monuteaux MC. Outcomes of nonoperative management of uncomplicated appendicitis. Pediatrics. 2017; 140(1):e20170048.
3. Alyamani AS, Bamatraf FF. Prevalence and Seasonality of Acute Appendicitis Among Patients Registered at Ibn-Sina General Hospital in Al-Mukalla, Yemen. HUJNAS. 2018;15(1):33-39.
4. Hsu YJ, Fu YW, Chin T. Seasonal variations in the occurrence of acute appendicitis and their relationship with the presence of fecaliths in children. BMC Pediatr. 2019;19(1):443.
5. Mohamed I, Chan S, Bhangu A, Karandikar S. Appendicitis as a manifestation of colon cancer: should we image the colon after appendicectomy in patients over the age of 40 years?. Int J Colorectal Dis. 2019;34(3):527-531.
6. Bar?æ?k CC, Bener A. Predictors risk factors for acute complex appendicitis pain in patients: Are there gender differences? J Family Med Prim Care. 2020;9(6):2688-92.
7. Nicole M, Desjardins MP, Gravel J. Bedside sonography performed by emergency physicians to detect appendicitis in children. Acad Emerg Med. 2018;25(9):1035-1041.
8. Yang Y, Guo C, Gu Z, Hua J, Zhang J, Qian S, et al. The global burden of appendicitis in 204 countries and territories from 1990 to 2019. Clin Epidemiol. 2022;14:1487-1499.
9. Körner H, Söndenaa K, Söreide JA, Andersen E, Nysted A, Lende TH, et al. Incidence of acute nonperforated and perforated appendicitis: age-specific and sex-specific analysis. World J Surg. 1997;21(3): 313-7.
10. Schildberg CW, Reissig K, Hunger R, Paasch C, Stillger R, Mantke R. Diagnostic, therapy and complications in acute appendicitis of 19,749 cases based on routine data: a retrospective multicenter observational study. J Clin Med. 2022;11(15):4495.
11. Parsons C, Shapiro NI, Cooper R, Tichter A, Morris A, Wolfe B, et al. Patient factors associated with appendectomy within 30 days of initiating antibiotic treatment for appendicitis. JAMA surg. 2022; 157(3):e216900.
12. Butt MQ, Chatha SS, Ghumman AQ, Farooq M. RIPASA score: a new diagnostic score for diagnosis of acute appendicitis. J Coll Physicians Surg Pak. 2014;24(12):894-7.
13. Abu Foul S, Egozi E, Assalia A, Kluger Y, Mahajna A. Is early appendectomy in adults diagnosed with acute appendicitis mandatory? A prospective study. World J Emerg Surg. 2019;14:2.
14. Avanesov M, Wiese NJ, Karul M, Guerreiro H, Keller S, Busch P, et al. Diagnostic prediction of complicated appendicitis by combined clinical and radiological appendicitis severity index (APSI). Eur Radiol. 2018;28(9):3601-3610.
15. Syed S, Naji H. A retrospective analysis of acute appendicitis in children treated with laparoscopic appendectomies at a single center in Dubai, UAE. Dubai Med J. 2021;4(3):225-30.
16. Crocker C, Akl M, Abdolell M, Kamali M, Costa AF. Ultrasound and CT in the diagnosis of appendicitis: accuracy with consideration of indeterminate examinations according to STARD guidelines. AM J ROENTGENOL. 2020;215(3):639-44.
17. Baghdadi MA, Metwalli AE, Abdelhamid MI. Preoperative laboratory tests as predictors of complicated appendicitis. EGYPT J SURG. 2019;38(3):535-41.
18. Potey K, Kandi A, Jadhav S, Gowda V. Study of outcomes of perforated appendicitis in adults: a prospective cohort study. Ann Med Surg (Lond). 2023;85(4):694-700.
19. Weinandt M, Godiris-Petit G, Menegaux F, Chereau N, Lupinacci RM. Appendicitis is a severe disease in elderly patients: a twenty-year audit. JSLS. 2020;24(3):e2020.00046.
20. Thomas JO. Acute appendicitis in Buraidah, Saudi Arabia. Cent Afr J Med. 1998;44(7):176-8.
21. Mungadi IA, Jabo BA, Agwu NP. A review of appendicectomy in Sokoto, North-western Nigeria. Niger J Med. 2004;13(3):240-3.
22. Kariya A, Krutsri C, Singhatas P, Sumritpradit P, Thampongsa T, Lertsitthichai P, et al. Incidence of complicated appendicitis during the COVID-19 pandemic: A systematic review and meta-analysis. Int J Surg Open. 2022;45:100512.
23. Scheijmans JC, Borgstein AB, Puylaert CA, Bom WJ, Bachiri S, van Bodegraven EA, et al. Impact of the COVID-19 pandemic on incidence and severity of acute appendicitis: a comparison between 2019 and 2020. BMC Emerg Med. 2021;21(1):61.
24. Gignoux B, Blanchet MC, Lanz T, Vulliez A, Saffarini M, Bothorel H, et al. Should ambulatory appendectomy become the standard treatment for acute appendicitis? World J Emerg Surg. 2018;13:28.
25. Oguntola AS, Adeoti ML, Oyemolade TA. Appendicitis: Trends in incidence, age, sex, and seasonal variations in South-Western Nigeria. Ann Afr Med. 2010;9(4):213-7.
26. Noudeh YJ, Sadigh N, Ahmadnia AY. Epidemiologic features, seasonal variations and false positive rate of acute appendicitis in Shahr-e-Rey, Tehran. Int J Surg. 2007;5(2):95-8.
27. Ohene-Yeboah M, Abantanga FA. Incidence of acute appendicitis in Kumasi, Ghana. West Afr J Med. 2009;28(2):122-5.
28. Al-Omran M, Mamdani MM, McLeod R. Epidemiologic features of acute appendicitis in Ontario, Canada. Can J Surg. 2003;46(4):263-8.
29. Albahadili MA. Study of the effect of age, gender and seasonal variation on appendicitis in Azizyah-Iraq. Al-Kufa University Journal for Biology. 2016;8(2):334-341.
Full Text Sources:
Abstract:
Views: 5514

For Authors
Journal Subscriptions

Dec 2025
Supplements
Instructions for authors
Online submission
Contact
e-ISSN: 2601 - 1700 (online)
ISSN-L: 2559 - 723X
Journal Abbreviation: Surg. Gastroenterol. Oncol.
Surgery, Gastroenterology and Oncology (SGO) is indexed in:
- SCOPUS
- EBSCO
- DOI/Crossref
- Google Scholar
- SCImago
- Harvard Library
- Open Academic Journals Index (OAJI)
Surgery, Gastroenterology and Oncology (SGO) is an open-access, peer-reviewed online journal published by Celsius Publishing House. The journal allows readers to read, download, copy, distribute, print, search, or link to the full text of its articles.
Time to first editorial decision: 25 days
Rejection rate: 61%
CiteScore: 0.2

Meetings and Courses in 2025
Meetings and Courses in 2024
Meetings and Courses in 2023
Meetings and Courses in 2022
Meetings and Courses in 2021
Meetings and Courses in 2020
Meetings and Courses in 2019
Verona expert meeting 2019

Surgery, Gastroenterology and Oncology applies the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits readers to copy and redistribute the material in any medium or format, remix, adapt, build upon the published works non-commercially, and license the derivative works on different terms, provided the original material is properly cited and the use is non-commercial. Please see: https://creativecommons.org/licenses/by-nc/4.0/
Publisher’s Note:
The opinions, statements, and data contained in article are solely those of the authors and not of Surgery, Gastroenterology and Oncology journal or the editors. Publisher and the editors disclaim responsibility for any damage resulting from any ideas, instructions, methods, or products referred to in the content.
 IASGO Society News
IASGO Society News