Surgery, Gastroenterology and Oncology

|
|
Background: Laparoscopic extra-levator abdomino-perineal excision (eLAPE) performed in the prone position has shown potential benefits for local recurrence and metastasis rates by reducing intraoperative perforation and positive circumferential resection margin outcomes.
Materials and Methods: Short-term results of Laparoscopic Extra-levator abdomino-perineal excision in the prone position in the treatment of low rectal cancer from December 2018 to June 2023, with 45 patients underwent eLAPE.
Results: The median age was 68 years. On average, tumors were 1.6 cm from the anal margin. The circumferential resection margin positivity rate was 28.9%, with a mean of 16.7 harvested lymph nodes and 1.6 positively detected nodes. T3 staging accounted for 68.9% of cases. Importantly, no intraoperative perforations occurred. Main postoperative complications involved the perineal incision, like bleeding and infection. The mean operation time was 258 minutes, with 73 minutes for perineal excision. A statistically significant difference in circumferential resection margin positivity existed between T2 and T3 grades (p=0.009). Conclusion: eLAPE for the treatment of low rectal cancer in the prone position has reduced the complications (IOP, CRM) rate.
Introduction
Rectal cancer is a prevalent malignant disease of the digestive system, and its treatment involves various modalities, with surgical intervention being the cornerstone of curative therapy (1,2). Surgical treatment often encounters numerous challenges, particularly in cases of low rectal cancer where preserving the patient's sphincter function is sometimes unfeasible due to the tumour's ultralow location or invasion into the external sphincter complex or the anal levator muscle (1,3).
Despite the fact that the first perineal rectal resection was performed by William Ernest Miles and established as a standard procedure for low rectal cancer over a century ago, it remains the most effective method for treating this type of cancer (4). In 1982, Richard John Heald introduced the technique of total mesorectal excision (TME), and the importance of circumferential resection margins (CRM), proposed by Philip Quirke in 1986, has contributed to reducing local recurrence rates and increasing five-year survival rates (5). However, the TME technique is only highly effective for anterior resection, and for perineal rectal resection, the recurrence rate remains high at 20% compared to anterior resection of the same stage (6-10).
The high rate of local recurrence or metastasis is attributable to various factors, including anatomical considerations related to the pelvic floor and this segment of the rectum, as well as the stage (T) of the tumour (1,3,11-13). In this portion of the rectum, there is no surrounding mesentery, and the surgical indication is for very low tumours, with margins up to 3-4 cm from the anal verge (7,13,14). Consequently, conventional dissection involves dissecting from the abdominal phase downward to the levator muscle, with the dissecting plane being closely adjacent to the rectum, thus limiting the acquisition of surrounding tissue. This often results in a waist-shaped sample at the tumour site, increasing the likelihood of cancer cell involvement in the circumferential resection margin (CRM). To mitigate this limitation, Torbjörn Holm and Philip Quirke improved the method by obtaining more tissue around the tumour through Extra-levator abdomino-perineal excision in a prone position (5,15-18). This approach offers several advantages, such as improved visibility for the surgeon and assistant, acquisition of more tissue around the tumour, and a reduced risk of intraoperative complications. Collectively, these factors contribute to a decreased risk of local recurrence or distant metastasis and enhance the overall survival rate.
Beginning in late 2018, the Can Tho University of Medicine and Pharmacy Hospital commenced the implementation of the Extra-levator abdomino-perineal excision procedure. This study aims to evaluate the relationships between CRM and recurrence, stage T, and tumour position, as well as to assess the technique of laparoscopic Extra-levator abdomino-perineal excision in the prone position for the treatment of low rectal cancer.
Materials and Methods
Methods of data collection and evaluation
Patients diagnosed with low rectal cancer were identified based on histopathological analysis (Invasive tumor in the levator muscles, fat of the ischiorectal fossa - rectum or perianal skin, perforation of the tumor with abscess or fistula in the ischiorectal fossa - rectum). The distance to the lower border of the tumour was determined via digital rectal examination or colonoscopy, and the tumour’s location on the rectal wall was mapped. Hemodynamic status was assessed during the patient's prone position, along with operating time, perineal excision time, oncological outcomes, tumour characteristics, CRM status, and lymph node status. Surgical results were monitored for complications during and after the operation, colostomy, and perineal wound condition.
The study was conducted on patients diagnosed with early-stage (I-III) rectal cancer who underwent laparoscopic Miles' procedure with perineal excision in the prone position, or stage I disease with T2 tumors accompanied by uncontrolled weight loss or no longer eligible for local excision. However, the study excluded patients who underwent laparoscopic Miles' procedure with perineal excision in the prone position but required open conversion or exploration due to distant metastases; patients with rectal cancer who received neoadjuvant chemoradiotherapy; patients with recurrent rectal cancer or synchronous cancers in two organs; and those with a history of lower abdominal cancer surgery, such as ovarian, cervical, uterine, or bladder cancer.
Surgical technique
Prior to the implementation of this technique, the surgeons performing the procedures in this study had over 15 years of experience in colorectal surgery and underwent additional training at the surgical center of the University of Leeds.
During the abdominal stage, the patient was placed in a supine position for laparoscopic exploration to assess tumour location, extent of invasion, and the presence of lymph node and liver metastases. Dissection exposed the inferior mesenteric artery, followed by lymph node dissection, ligation of the inferior mesenteric artery, and mobilization of the rectosigmoid colon to facilitate total mesorectal excision (TME). Anteriorly, dissection extended to the seminal vesicles in men and the cervix in women. Posteriorly, dissection reached the top of the coccyx, avoiding excessive depth to prevent a waisted shape, which minimizes the risk of retaining residual tumour cells, as indicated by an increased CRM (+) rate. A sigmoid colostomy was created at the left iliac fossa, and the patient was repositioned into the prone position.
During the perineal stage, the buttocks were covered with wide tape to expose the perineal area. Purse-string sutures were placed around the anus approximately 2 cm from the anal margin. The skin around the anus was incised from the top of the coccyx. Subcutaneous fat was cut to expose the anal levator muscle. The levator muscle was dissected at the top of the coccyx, extending into the abdominal cavity. The wide levator muscle was removed, and the rectum was extracted in reverse. At this stage, surrounding structures such as the prostate or the posterior vaginal wall were distinctly exposed. The wide levator muscle and the anorectal complex sphincter were removed from the perineum. The perineal excision was sutured using autologous tissue or mesh in cases of insufficient tissue. Specimens were fixed for lymph node evaluation and histopathological analysis.
Statistical analysis
The data were encoded, processed, and analyzed using SPSS 20.0 (IBM Corp., New York, USA) software for statistical analysis. Descriptive statistics summarized quantitative variables by means and standard deviations (for normally distributed variables), medians (for non-normally distributed variables), and frequencies and percentages for categorical variables. For categorical variables, the chi-square test with Fisher's exact test as a correction was used, and for continuous variables, the t-test was employed. Univariate analysis was conducted to identify variables associated with treatment outcomes. Variables significantly related to treatment outcomes (p <0.05 through univariate analysis) were included in multivariate analysis to adjust OR (Odds Ratio) values and determine confidence intervals. Multivariate logistic regression was used to identify factors related to treatment outcomes.
Research ethics
The study was conducted with integrity and diligence, aiming to enhance public health by preventing and managing diseases within the community. Ethical considerations for this study were approved by the Scientific Review Committee of Can Tho University of Medicine and Pharmacy, under code 022/H??-PCT, and in accordance with the 2013 Helsinki Declaration. All research participants were provided with detailed explanations regarding the purpose and content of the study, and they voluntarily agreed to participate and collaborate throughout the research process.
Participants had the right to refuse participation or withdraw from the study at any stage.
Histopathology
Specimens were fixed and immersed in a solution of 10% neutral formalin. Lymph nodes, T stage, CRM, and tissue differentiation were evaluated. The pathologist was trained by Professor Philip Quirke at St James's University Hospital, Leeds, United Kingdom.
Results
Between December 2018 and June 2023, 45 cases of laparoscopic Extra-levator abdomino-perineal excision met the selection criteria. The mean age of patients was 64 years, ranging from 38 to 96 years. Our study included 24 female patients, representing 53.3% of the total cases. Notably, rectal cancer in individuals under 40 years old constituted 6.6% of the cases. The average duration of the abdominal phase of the surgery was 161 minutes (ranging from 80 to 300 minutes), while the average time for perineal excision was 72 minutes (ranging from 28 to 110 minutes). There were no instances of intraoperative complications (IOP). Furthermore, no signs of hyperpressure, such as facial edema or conjunctival congestion, were observed in relation to the prone position.
Postoperative complications were primarily associated with the perineal incision. There was one case of postoperative bleeding, and perineal incision infections accounted for 17.8% of the cases. Additionally, two cases exhibited sinus fluid accumulation in the perineal area. The average postoperative hospital stay was 8.4 days, with a range of 6 to 24 days.
Histologically
Adenocarcinoma was present in 100% of the cases. The majority of tumours were moderately
differentiated, comprising 84.4% of the cases, followed by poorly differentiated tumours at 13.3% and well-differentiated tumours at 2.2%. The average distance from the anal verge to the lower border of the tumour was 1.6 cm, with a range of 0 to 4 cm (fig. 1).
Figure 1 - Extra-levator abdomino-perineal excision, (a) Pull the rectum reverse with the tumour, (b) perineal incision after anorectal resection, (c) The specimen has a cylindrical shape, (d) The postoperation specimen harvest and histopathology.
(Source: Can Tho University of Medicine and Pharmacy Hospital)

Table 1 - Postoperative stages

Regarding T staging, stage T3 was the most common, representing 71.1% of the cases, while stage T2 accounted for 28.9%. In terms of overall disease staging, stage 3 was predominant, comprising 46.7% of the cases, with stage 2 representing 33.3% (table 1).
Clinically, tumours located on the anterior wall, right or left halves, or annular tumours were related to the regional rectum having little connective tissue and no mesentery (fig. 2).
Figure 2 - Anterior part, the area above the extraperitoneal levator muscle without surrounded mesentery.
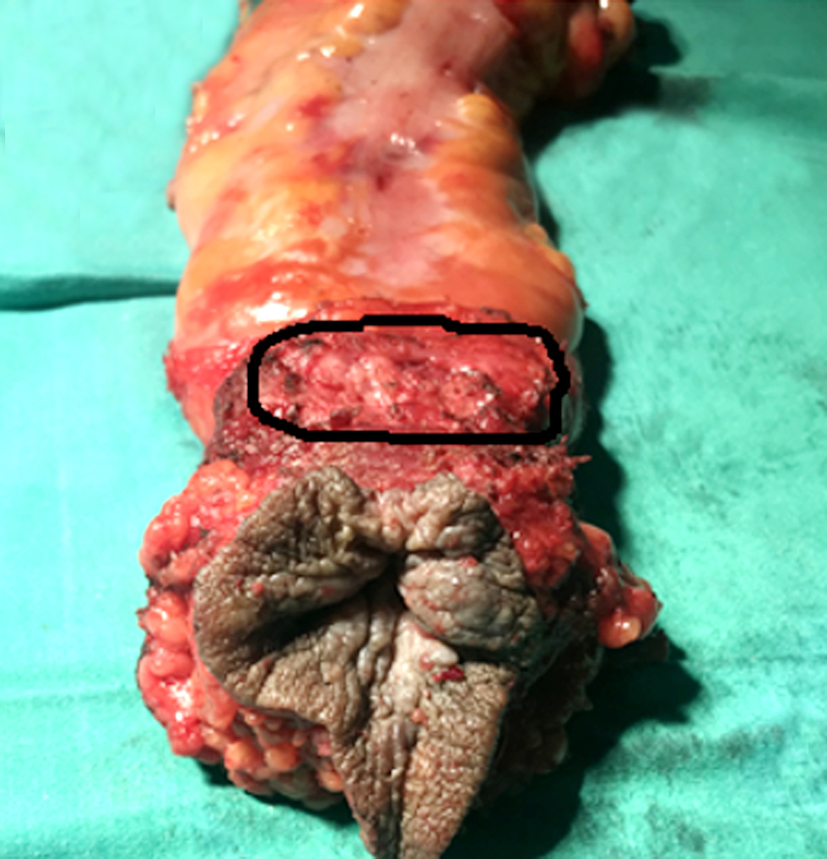
The average number of harvested lymph nodes was 16, ranging from 12 to 24, with an average of 1.6 lymph nodes showing metastasis. Circumferential resection margin (CRM) positivity was observed in 28.9% of the cases. There were 32 cases with negative CRM, accounting for 71.1%. Achieving a negative surgical margin in this dissection is also an important factor. Several studies have shown that local recurrence or distant metastasis is associated with CRM (+). In our patient group, the CRM (+) rate was 28.9%. We found that the T3 stage accounted for a high proportion at 71.1% in the study group (table 2). The relationship between CRM results and T stage in the study sample is as follows: Stage T2 had no CRM (+) cases, all were CRM (-). Stage T3 had 40.6% CRM (+) cases, while 59.4% were CRM (-). There was a statistically significant difference in CRM (+) results between the T2 and T3 stages (p=0.009).
Table 2 - Corelations between CRM with Recurrence, Stage T and Tumour positions.

Table 3 - Postoperative complications

Wound infection is a common complication, and when an infection causes delays in wound healing, it is classified as grade II or higher. In our study group, grade I infections accounted for 6.7%, while grade II infections accounted for 8.9%. There was one case of bleeding after perineal excision, comprising 2.2% of the cases (table 3).
The overall survival rates at 1 year, 2 years, and 3 years were 100%, 95.2%, and 85.7% respectively. At the end of the study period, the rates of local recurrence, distant metastasis, and mortality were 6.6%, 6.6%, and 4.4% respectively.
Discussions
Laparoscopic Extra-levator abdomino-perineal excision in the prone position offers numerous advantages for both the surgeon and the assistant, as observed in our study. The surgical procedure is more convenient, and the assistant does not encumber or spread over the patient's legs, as may occur in the supine position (19,20). Applying the prone position for perineal resection: it provides good visualization, a wide surgical field, and does not obstruct the assistant surgeon, allowing for more extensive dissection around the tumor. There were no cases of increased pressure on the lower body (facial swelling, eye issues, or compression of the knees, chest, etc.). Hemodynamic changes with position changes were also negligible.
One of the challenging stages of dissection is the downward (backward) change of the anterior half of the rectum. However, in the prone position, direct vision with the light of standard operating lights eliminates the need for posterior lighting, as required in the supine position (21). Dissecting the rectum away from the prostate gland in men and the posterior vaginal wall in women can be difficult and requires meticulous and time-consuming surgery to avoid damaging surrounding structures or causing intraoperative perforation (IOP). The Extra-levator perineal excision in the prone position provides direct visibility, simplifying dissection and preserving more tissue around the tumour, thereby reducing the rate of CRM (+) (15,20). Performing this phase in the supine position places this area above, making it difficult to observe, and sometimes the surgeon may have to turn their head to dissect properly, possibly leading to perforation or damage to the prostate, posterior vaginal wall, or urethra. However, the prone position provides a larger surgical field, aiding in better bleeding control and significantly reducing blood loss during surgery (22).
The prone position, however, has the disadvantage of increasing pressure in the lower half of the body and may lead to complications such as facial edema (21,22). In our study, we observed no cases of facial or eye edema. Hyperpressure often emerges in spine surgery groups due to extended operating times, potentially causing the aforementioned complications. In our study, the average operative duration for perineal excision was 72 minutes (28-115). The average time for changing positions was 13 minutes (5-30) due to the use of new technology, and the training team was still in the process of becoming proficient and synchronized in position changing, leading to preparation time fluctuations of 20-30 minutes. However, later on, the time to change positions reduced significantly. According to the author, operations lasting less than 6 hours seldom result in complications (22).
These results indicate that the eLAPE procedure for cylindrical tumors may result in a lower risk of intra-operative perforation compared to the classical Miles operation, and can potentially improve oncological outcomes, as well as reduce intraoperative blood loss and perforation. The study has provided compelling evidence that eLAPE should be considered for low-lying tumors.
Intraoperative perforation
Intraoperative perforation is another factor associated with recurrence related to bowel or tumour perforation during the operation. Our IOP result was 0%, despite the majority of tumours being stage T3. This demonstrates the advantage of performing Extra-levator abdomino-perineal excision. However, our study’s sample size was relatively small, and the statistical analysis may not be as accurate as in the studies mentioned above (23,24).
Relationship between CRM and tumour location, location and recurrence We divided the rectal locations into anterior (10h-2h) and posterior (3h-9h). The anterior location includes tumours on the anterior wall, either on the right or left halves, or annular tumours directly contacting the prostate glands in males or the posterior vaginal wall in females. The posterior location is surrounded by the mesentery, resulting in a higher negative rate for CRM (8). Around 88.9% of tumours were over 3 cm in vertical size (measured from the lower border to the upper edge of the tumour). Simultaneously, tumours with a height greater than 3 cm indicate that the tumour is located beyond the upper border of the levator ani muscle, and when evaluating CRM, the combination of tumour location and size indicates a high risk of a positive rate. Following the study of Norbert Garcia-Henriquez, it is suggested that the position may influence overall oncologic outcomes (19). According to Suk Hawn Lee et al., anterior tumours tend to be more advanced and, in male patients at least, have a higher risk of recurrence and death compared to tumours in other locations. However, upon analyzing the statistics, we found that the correlation between CRM and tumour location indicated that CRM (+) rates were 23.1% of cases in the posterior position, 27.3% in the anterior position, 40% in the annular form, and 27.3% in the remaining right and left half positions. The risk of CRM (+) in posterior, anterior, and annular positions was 2.22, 1.25, and 1.25 times higher compared to the posterior position. However, statistically, these differences were not significant, similar to the results of other authors.
Our study results reveal that in the "anterior" position group, there were 27.3% cases with CRM (+), while in the "posterior" position group there were 23.1%. In the "annular" position group, our study recorded 40% of cases with CRM (+), while in the "right half, left half" positions group, there were 27.3% cases with CRM (+). However, there was no significant difference in surgical outcomes of the groups when compared with the "anterior position" group (p>0.05).
Analysis of recurrence related to CRM status
When analyzing the location of recurrence related to CRM (+) and CRM (-) status, the CRM (-) group had 32 cases, accounting for 71.1%: 1 case of lung metastasis accounted for 3.1%, and 1 case of liver and lung metastasis accounted for 3.1%; there were no local cases. In the CRM (+) group, there were 13 cases, accounting for 28.9%: recurrence in the perineum area was 3 cases, accounting for 23.1%, and liver and lung metastasis was 1 case, accounting for 7.7%.
The results showed that the CRM (+) group had a higher recurrence in the perineum than the CRM (-) group. When conducting statistical analysis to evaluate the correlation between overall recurrence status and circumferential margin status, we observed that in the CRM (+) group, there was a recurrence rate of 30.8%, whereas in the CRM (-) group, the recurrence rate was 6.3%. The statistical analysis indicates that the CRM (+) group has a higher risk of overall recurrence compared to the CRM (-) group, with an Odds Ratio (OR) of 6.67, and this difference was statistically significant (p=0.049).
Results of surgery
Performing Laparoscopic Extra-levator Abdomino-perineal Excision (eLAPE) within the abdominal cavity is generally straightforward due to the tumour’s location outside the peritoneum, leading to minimal complications during surgery. However, the perineal excision necessitates the extensive removal of a significant amount of tissue, resulting in a considerable defect in the perineal area and numerous complications associated with this wound. The study by Galal El-Gazzaz, M.D., et al., reported an overall wound complication rate of 16.2% (25).
Regarding postoperative follow-up over 22 months, there were two cases of perineal fluid sinuses that emerged more than one year post-surgery, diagnosed through ultrasound and CT scan imaging of the pelvis.
Limitations of the study
Despite the valuable insights and advantages garnered from this study on Laparoscopic Extra-Levator Abdomino-Perineal Excision, several limitations must be acknowledged. One limitation is the relatively small sample size, which may limit the generalizability of the findings. Larger sample sizes are necessary to strengthen the statistical power and draw more robust conclusions (1,12). Additionally, the study was conducted solely at a single medical center, which may introduce biases and limit the diversity of patient populations and clinical practices considered. Moreover, the 22-month follow-up period of our study might not provide a complete picture of long-term oncologic outcomes. Longer follow-up durations are needed to accurately assess recurrence rates and survival. One of the limitations of the diagnostic process in this study was the non-routine use of MRI for all cases, due to the relatively high cost compared to the financial means of Vietnamese patients. However, we believe that preoperative pelvic MRI should be performed to assess the extent of tumor invasion and stage rectal cancer, as well as to evaluate the circumferential resection margin (CRM) prior to surgery, in order to plan for neoadjuvant chemoradiotherapy when necessary.
Implications
The study's findings underscore the benefits of Laparoscopic Extra-levator Abdomino-perineal Excision (eLAPE) for improved rectal cancer resection. Surgeons should consider adopting eLAPE to enhance outcomes and minimize complications. Clear circumferential resection margins are crucial, correlating with tumour stage and affecting recurrence rates. This emphasizes the need for meticulous resection. The study guides patient selection, particularly for sphincter preservation cases, potentially leading to better functional outcomes. Additionally, insights into prone positioning impact postoperative complications, aiding in safer surgeries and standardized protocols.
Further study
To enhance the generalizability of our findings, multi-center studies with larger and more diverse samples are needed. Extending the follow-up duration to explore longer-term outcomes over five years would provide comprehensive insights. Comparative studies between eLAPE and other techniques are valuable for assessing benefits. Advanced statistical methods could offer deeper insights by controlling for confounders. Integrating patient-reported outcomes and quality of life assessments would provide a holistic view. Such research would refine surgical approaches, optimize patient care, and contribute to improved outcomes in the treatment of low rectal cancer.
Conclusions
Laparoscopic Extra-levator Abdomino-perineal Excision (eLAPE) performed in the prone position offers several advantages, including enhanced anatomical visibility. This procedure is favorable for dissection to obtain more tissue around the tumour. The correlation between CRM (+) and the T stage is evident, and while perineal wound infection complications exist, they are manageable at a moderate level. The presence of CRM (+) correlates with the T stage, while the complication rate of perineal wound infection is relatively moderate. Recurrence rates after a 22-month period remain notable. For advanced low rectal cancer patients, especially those requiring sphincter preservation and categorized as stage T3 or T4, this procedure emerges as a favorable choice.
Contribution
All authors have read and agreed to the published version of the manuscript.
Acknowledgement
We acknowledge the cooperation and support of some patients in Hospital of Can Tho University of Medicine and Pharmacy. We also thank you for the support from Can Tho University of Medicine and Pharmacy.
Funding: None to declare.
References
1. Bray F, Laversanne M, Sung H, Ferlay J, Siegel RL, Soerjomataram I, et al. Global cancer statistics 2022: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2024;74(3):229-263.
2. Sugimoto K, Takahashi H, Yuki T 2nd, Irie T, Kawaguchi M, Kobari A, et al. Positive Circumferential Resection Margin in Rectal Cancer Is a Robust Predictor of Poor Long-term Prognosis With Clinico-pathological Bias Between Groups Compensated by Propensity-score Matching Analysis. Anticancer Res. 2023;43(8):3623-3630.
3. Wang C, Gan L, Gao Z, Shen Z, Jiang K, Ye Y. Young adults with colon cancer: clinical features and surgical outcomes. BMC Gastroenterology. 2023;23(1):192.
4. Miles WE. A method of performing abdomino-perineal excision for carcinoma of the rectum and of the terminal portion of the pelvic colon (1908). CA Cancer J Clin. 1971;21(6):361-364.
5. Quirke P, Durdey P, Dixon MF, Williams NS. Local recurrence of rectal adenocarcinoma due to inadequate surgical resection. Histopathological study of lateral tumour spread and surgical excision. Lancet. 1986;2(8514):996-999.
6. Chardalias L, Papaconstantinou I, Gklavas A, Politou M, Theodosopoulos T. Iron Deficiency Anemia in Colorectal Cancer Patients: Is Preoperative Intravenous Iron Infusion Indicated? A Narrative Review of the Literature. Cancer Diagn Progn. 2023;3(2): 163-168.
7. Wilkins S, Yap R, Mendis S, Carne P, McMurrick PJ. Surgical Techniques for Abdominoperineal Resection for Rectal Cancer: One Size Does Not Fit All. Front Surg. 2022;9:818097.
8. Park HM, Song O, Lee J, Lee SY, Kim CH, Kim HR. Impact of circumferential tumor location of mid to low rectal cancer on oncologic outcomes after preoperative chemoradiotherapy. Ann Surg Treat Res. 2022;103(2):87-95.
9. Eseme EA, Scampa M, Viscardi JA, Ebai M, Kalbermatten DF, Oranges CM. Surgical Outcomes of VRAM vs. Gracilis Flaps in Vulvo-Perineal Reconstruction Following Oncologic Resection: A Proportional Meta-Analysis. Cancers (Basel). 2022;14(17):4300.
10. Varela C, Kim NK. Surgical Treatment of Low-Lying Rectal Cancer: Updates. Ann Coloproctol. 2021;37(6):395-424.
11. ?ermanovi? A, Radovanovi? Z, Luki? D, ?uri? M, Kresoja M, Golijanin D. Extralevator abdominoperineal excision for low rectal cancer: oncological outcome after five-year follow-up. S Afr J Surg. 2021;59(4):164-168.
12. Mroczkowski P, Kim S, Otto R, Lippert H, Zajdel R, Zajdel K, et al. Prognostic Value of Metastatic Lymph Node Ratio and Identification of Factors Influencing the Lymph Node Yield in Patients Undergoing Curative Colon Cancer Resection. Cancers (Basel). 2024;16(1):218.
13. Peng W, Qiao H, Mo L, Guo Y. Progress in the diagnosis of lymph node metastasis in rectal cancer: a review. Front Oncol. 2023;13: 1167289.
14. Mroczkowski P, Dziki ?, Vosikova T, Otto R, Merecz-Sadowska A, Zajdel R, et al. Rectal Cancer: Are 12 Lymph Nodes the Limit? Cancers (Basel). 2023;15(13):3447.
15. Holm T. Abdominoperineal Excision: Technical Challenges in Optimal Surgical and Oncological Outcomes after Abdominoperineal Excision for Rectal Cancer. Clin Colon Rectal Surg. Nov 2017;30(5):357-367. doi:10.1055/s-0037-1606113
16. Jörgren F, Johansson R, Damber L, Lindmark G. Oncological outcome after incidental perforation in radical rectal cancer surgery. Int J Colorectal Dis. 2010;25(6):731-740.
17. Quirke P, Steele R, Monson J, Grieve R, Khanna S, Couture J, et al. Effect of the plane of surgery achieved on local recurrence in patients with operable rectal cancer: a prospective study using data from the MRC CR07 and NCIC-CTG CO16 randomised clinical trial. Lancet. 2009;373(9666):821-8.
18. Holm T, Ljung A, Häggmark T, Jurell G, Lagergren J. Extended abdominoperineal resection with gluteus maximus flap reconstruction of the pelvic floor for rectal cancer. Br J Surg. 2007;94(2):232-238.
19. Garcia-Henriquez N, Galante DJ, Monson JRT. Selection and Outcomes in Abdominoperineal Resection. Front Oncol. 2020; 10:1339.
20. Liu P, Bao H, Zhang X, Zhang J, Ma L, Wang Y, et al. Better operative outcomes achieved with the prone jackknife vs. lithotomy position during abdominoperineal resection in patients with low rectal cancer. World J Surg Oncol. 2015;13:39.
21. Roig-Vila JV, García-Armengol J, Bruna-Esteban M, Redondo-Cano C, Tornero-Ibáñez F, García-Aguado R. Operating position in colorectal surgery. The importance of the basics. Cir Esp. Oct 2009;86(4): 204-212.
22. Feix B, Sturgess J. Anaesthesia in the prone position. Continuing Education in Anaesthesia Critical Care & Pain. 2014;14(6):291-297.
23. Bülow S, Christensen IJ, Iversen LH, Harling H. Intra-operative perforation is an important predictor of local recurrence and impaired survival after abdominoperineal resection for rectal cancer. Colorectal Dis. 2011;13(11):1256-1264.
24. Eriksen MT, Wibe A, Syse A, Haffner J, Wiig JN. Inadvertent perforation during rectal cancer resection in Norway. Br J Surg. 2004;91(2):210-6.
25. El-Gazzaz G, Kiran RP, Lavery I. Wound complications in rectal cancer patients undergoing primary closure of the perineal wound after abdominoperineal resection. Dis Colon Rectum. Dec 2009; 52(12):1962-1966.
Full Text Sources:
Abstract:
Views: 3216

For Authors
Journal Subscriptions

Dec 2025
Supplements
Instructions for authors
Online submission
Contact
e-ISSN: 2601 - 1700 (online)
ISSN-L: 2559 - 723X
Journal Abbreviation: Surg. Gastroenterol. Oncol.
Surgery, Gastroenterology and Oncology (SGO) is indexed in:
- SCOPUS
- EBSCO
- DOI/Crossref
- Google Scholar
- SCImago
- Harvard Library
- Open Academic Journals Index (OAJI)
Surgery, Gastroenterology and Oncology (SGO) is an open-access, peer-reviewed online journal published by Celsius Publishing House. The journal allows readers to read, download, copy, distribute, print, search, or link to the full text of its articles.
Time to first editorial decision: 25 days
Rejection rate: 61%
CiteScore: 0.2

Meetings and Courses in 2025
Meetings and Courses in 2024
Meetings and Courses in 2023
Meetings and Courses in 2022
Meetings and Courses in 2021
Meetings and Courses in 2020
Meetings and Courses in 2019
Verona expert meeting 2019

Surgery, Gastroenterology and Oncology applies the Creative Commons Attribution Non Commercial (CC BY-NC 4.0) license, which permits readers to copy and redistribute the material in any medium or format, remix, adapt, build upon the published works non-commercially, and license the derivative works on different terms, provided the original material is properly cited and the use is non-commercial. Please see: https://creativecommons.org/licenses/by-nc/4.0/
Publisher’s Note:
The opinions, statements, and data contained in article are solely those of the authors and not of Surgery, Gastroenterology and Oncology journal or the editors. Publisher and the editors disclaim responsibility for any damage resulting from any ideas, instructions, methods, or products referred to in the content.
 IASGO Society News
IASGO Society News